Molluscum contagiosum (MC) is a common skin condition with a prevalence ranging from 5.1% and 11.5% in children aged 0 to 16 years.1 It is characterised by small dome-shaped bumps on the skin with a central white or “waxy” core. They can develop in any region of the skin but tend to spread in areas subject to friction. Although susceptibility to MC varies between individuals, children with chronic skin conditions such as atopic dermatitis are more likely to develop it. Inflammatory reactions are well-known manifestations of MC infection; however, there is a dearth of published data on their frequency, epidemiology and clinical spectrum.
We describe a series of 5 cases in children aged 4 to 10 years (Table 1), 3 of who had a previous diagnosis of atopic dermatitis. They presented to our emergency dermatology department with severely pruritic inflammatory lesions in the elbows and knees with acute onset in the past 48 to 72 hours. The patients did not have fever or any other general symptoms and had not taken any medication before the lesions appeared; however, they all previously consulted a physician due to MC (2 of them received no treatment, 2 were treated with 10% potassium hydroxide and 1 with cantharidin). The physical examination revealed pink-to-red oedematous papules involving the extensor surfaces of the extremities (Fig. 1), in 3 cases restricted to the knees and elbows. The eruption started when MC became inflamed, suggesting a possible association. Treatment consisted of topical or oral corticoids depending on the extent and degree of inflammation of the lesions. After 7 to 15 days of treatment, the lesions disappeared, as did the MC.
Characteristics of Gianotti-Crosti syndrome-like reactions in our five patients.
| Sex | Age | Medical history | Duration of MC previous to GCLRs | Clinical presentation | Areas involved | Treatment | GCLRs and time to resolution of MC | |
|---|---|---|---|---|---|---|---|---|
| Patient 1 | Female | 8 | Atopic dermatitis | 2 months | Pink to reddish oedematous papules | Elbows and knees | Oral corticosteroids | 2 weeks |
| Patient 2 | Female | 4 | Atopic dermatitis | 3 weeks | Millimetric papules | Elbows, buttocks and knees. | Topical corticosteroids | 1 week |
| Patient 3 | Male | 10 | Atopic dermatitis | 2 weeks | Reddish oedematous papules | Elbows and knees | Oral corticosteroids | 1 week |
| Patient 4 | Male | 4 | None | 1 month | Reddish pink lichenoid papules | Elbows | Topical corticosteroids | 2 weeks |
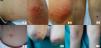
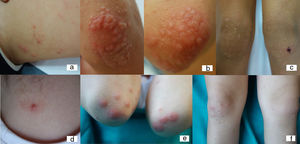
1- Patient 3. 10-year-old male with Gianotti-Crosti syndrome-like reaction to molluscum contagiosum. (1a) Inflamed MC lesions in the thigh. (1b) Inflammatory oedematous red papules on the elbows. (1c) Pink papules on the knees, Koebner response secondary to scratching.
2- Patient 1. 8-year-old female with Gianotti-Crosti syndrome-like reaction to molluscum contagiosum. (2a) Inflamed MC in the cervical area. (2b-c) Oedematous pink to red papules on the elbows and knees.
Inflammatory reactions secondary to MC infection are poorly studied, but they are common, frequently causing pruritus and pain. In many cases, there is local inflammation that may be mistaken for bacterial superinfection. In individuals with atopic dermatitis, MC lesions tend to appear in eczematous dermatitis areas. Less frequently, affected individuals may develop a severe inflammatory reaction consisting of a pruritic papular exanthem on the elbows and knees and known as Gianotti-Crosti syndrome-like reaction (GCLR).2–4 A recent retrospective study of 696 patients with MC found GCLRs in 34 patients (4.9% of cases): in 23 of them (67.6%) involving exclusively the extensor surfaces of the extremities, and in the remaining 12 (35.3%) restricted to the knees and/or elbows.5
Gianotti-Crosti syndrome-like reactions are characterised by lichenoid papules around the elbows, knees and buttocks. There is no association between the number of MC lesions and the development of GCLRs.5 This reaction may be present at the initial visit (50%) or 1 to 2 months after initiation of treatment of MC (38%), independently of the treatment received.5 In children, Gianotti-Crosti eruptions are usually associated with viral infections (EBV or hepatitis), with development of asymptomatic skin lesions usually preceded by a low-grade fever, sore throat or general discomfort. These patients experience a severe, intensely itchy inflammatory response to MC with development of these characteristic lesions, which in most cases is followed by resolution of MC within days or weeks.
Please cite this article as: Estébanez A, et al. Síndrome de Gianotti-Crosti-like secundario a Molluscum contagiosum. An Pediatr (Barc). 2020;93:49–50.