Group A Streptococcus (GAS), also known as Streptococcus pyogenes, is the most frequent causative agent in cases of bacterial pharyngitis in children and adolescents. Although it is not frequent, it can cause invasive infections (iGAS) with particularly severe presentations, such as sepsis, toxic shock, pneumonia, meningitis, osteoarticular infection, deep abscesses or necrotising fasciitis, which are frequently fatal.1–3
In December 2022, the government of the United Kingdom issued an alert warning of an unusual increase in the incidence of infections by S. pyogenes (chiefly tonsillitis and scarlet fever) and, simultaneously, of invasive infections with a significant mortality.4 Several countries in Europe soon reported similar increases in iGAS infections,5,6 and pneumonia is possibly the presentation whose incidence increased the most during this outbreak.7
However, this increasing trend in incidence was already apparent in the years preceding the SARS-CoV-2 pandemic, and had also been described in Spain.1 During the SARS-CoV-2, streptococcal infections and all other community-acquired viral and bacterial infections nearly disappeared, and in the 2022–2023 winter season there was a resurgence of all these infections in the paediatric population, which inspired the controversial concept of “immunity debt”. The obvious question is whether the incidence has increased for all forms of S. pyogenes infection or, on the contrary, there has been a shift in the circulating strains so that there are more virulent strains compared to previous years, or any other reason that may explain the phenomenon.
In Spain, infection by S. pyogenes is not a notifiable disease, even in the case of invasive infection, so it is not possible to make an accurate assessment of what has happened and is currently happening in our country. Although it does not make up for the lack of a national epidemiological surveillance system, we have the Paediatric GAS Network (PedGAS-net), an initiative of the Sociedad Española de Infectología Pediátrica (Spanish Society of Paediatric Infectious Diseases), which has been recording the cases of invasive infection since 2019 in a network of public hospitals throughout the country that currently includes 51 centres.
At the outset, some authors in the domestic literature spoke of a return to prepandemic trends,8 but, later, the same group based in Madrid calculated the incidence of GAS in relation to the total emergency department (ED) visits, and found an incidence of 22.85 cases per 1000 ED visits in the first semester of 2023, double the proportion found in 2022 (10.2 cases/1000 ED visits) and in 2019 (12.38 cases/1000 ED visits). The incidence of iGAS infection also increased in the same period, from 02 cases per 1000 ED visits in 2022 or 0.38 cases per 1000 ED visits in 2019, to nearly double in 2023, where the proportion reached 0.58 cases per 1000 ED visits9 (Fig. 1). The PedGas-Net analysed trends in iGAS infections, finding a substantial increase in late 2022 and early 2023, greater compared to the years before the pandemic,10 both in terms of frequency and severity. The increase in cases, which was also associated with a high proportion of pneumonia, was concurrent with a similar increase in respiratory tract infections by respiratory syncytial virus (RSV) and influenza, both in the United Kingdom and in Spain, with a high incidence of viral and bacterial coinfection10,11 (Fig. 2).
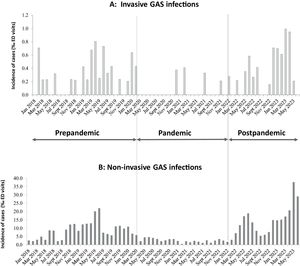
Infections by S. pyogenes in Hospital La Paz in the prepandemic period, during the pandemic and in the postpandemic period. Source: De Ceano-Vivas et al.9
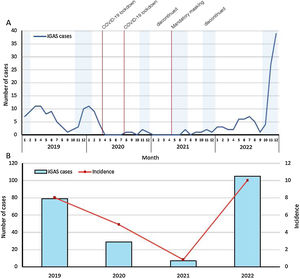
Children given a diagnosis of invasive infection by S. pyogenes in Spain between 2019 and 2022 (PedGas-Net). Source: Cobo-Vazquez et al.5
(A) Monthly case distribution. The red vertical lines indicate marked changes in public health control measures to prevent SARS-CoV-2 transmission. The blue bars represent the respiratory syncytial virus epidemic season in Spain.
(B) Annual absolute frequency and incidence of iGAS cases.
As regards the circulating strains, few studies have assessed this aspect to date, although the data currently available shows a similar strain distribution than reported in the prepandemic period, especially when it came to invasive infections,12 with a predominance of serotype M1, historically one of the most frequently involved, and an M1UK variant, particularly involved in cases manifesting with pneumonia. A study conducted in Spain through the collaboration of the Centro Nacional de Microbiología (CNM, National Centre of Microbiology) and PedGAS-net and sponsored by the CIBER (Centro de Investigacion Biomedica en Red) CIBERINFEC (One of the CIBER specific network), which has yet to be published, did not seem to identify new strains or great microbiological differences between mild and severe cases that could explain the recent outbreak. When it came to antibiotic resistance, it does not seem that resistance of S. pyogenes to any of the different antibiotics available could account for the severe cases. Resistance to penicillin has not been reported and even the collaborative study of the CNM-CIBERINFEC-PedGAS-net did not find evidence of an increased resistance to clindamycin that would explain more severe presentations in iGAS infections, in which this antibiotic is used as an adjuvant.
Last of all, we have to contemplate the hypothesis that the immune response of children could have been weakened by the isolation measures taken during the pandemic with the associated lack of exposure to infectious agents. This “immunity debt”, which would not correspond to an actual immune defect but rather to a large pool of susceptible naïve individuals, could have also played a role in the surge of all viral and bacterial infections in numbers far exceeding those of previous years. Viral and bacterial coinfection, a long-known phenomenon, could have created the perfect conditions for the emergence of this important outbreak which, although it is still too early to say, does not seem to be recurring with the same intensity in the 2023–2024 season.