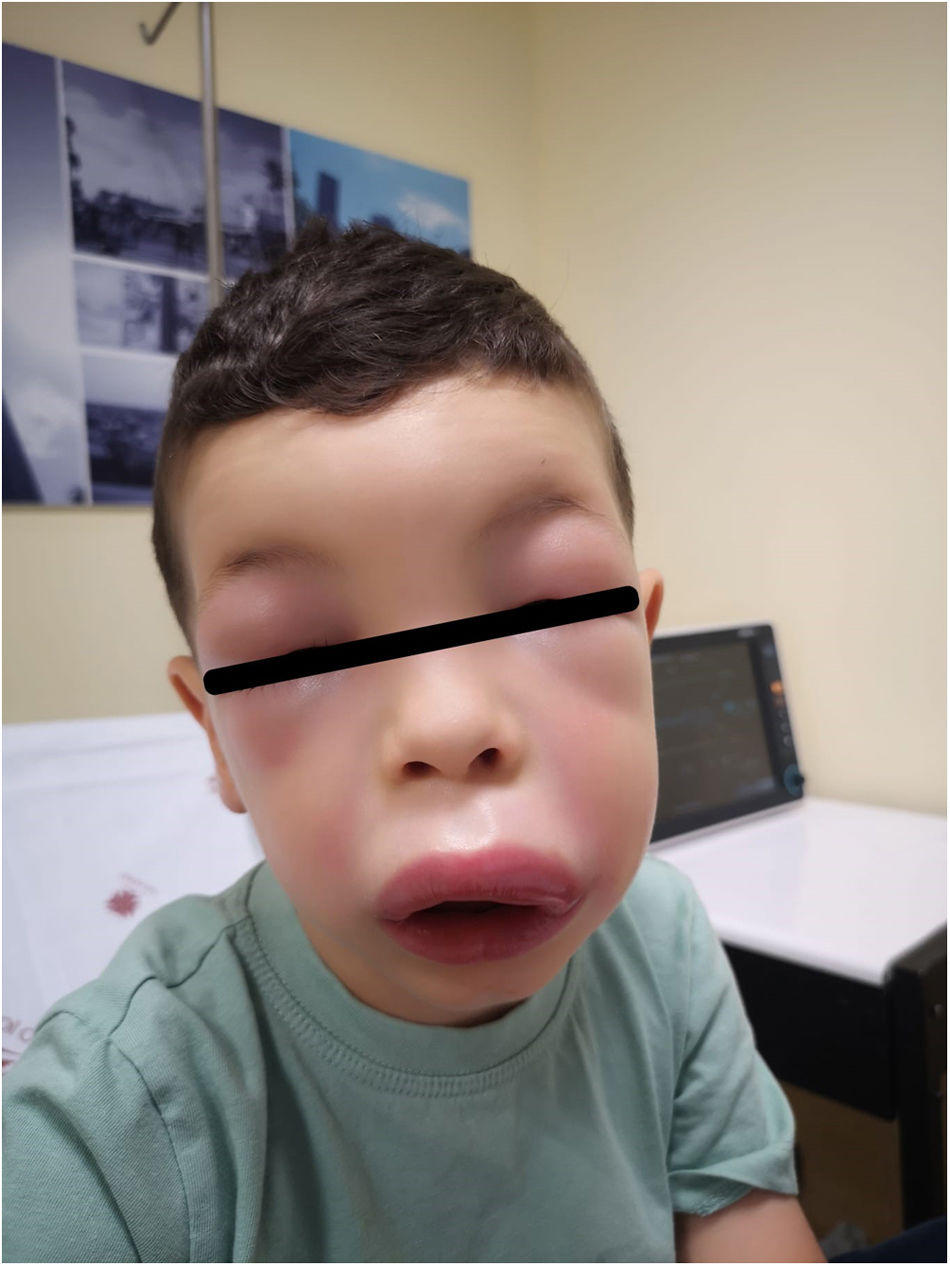
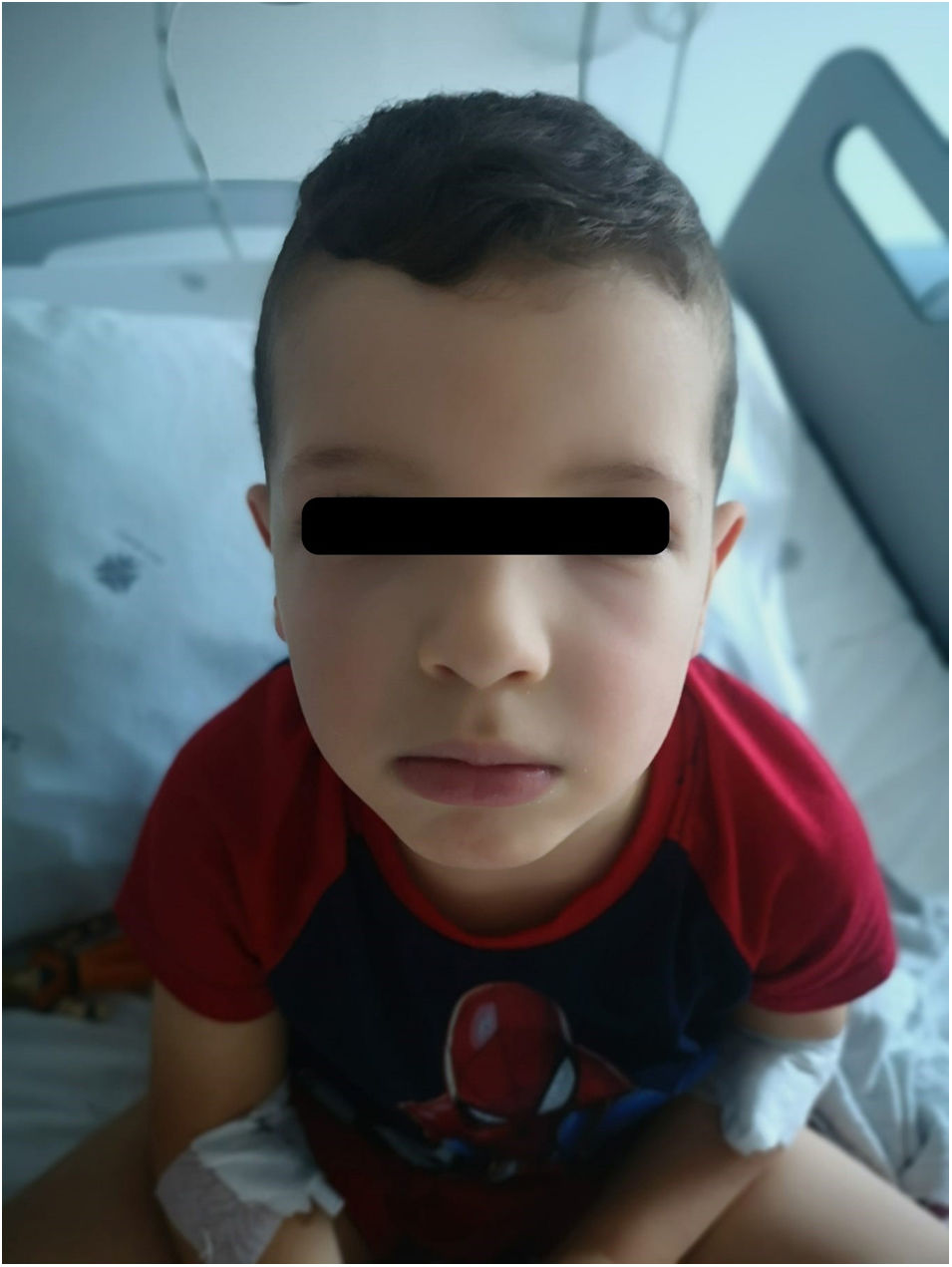
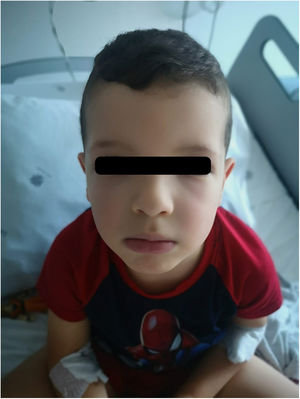
A boy aged 4 years presented to the emergency department (ED) with exuberant facial swelling of 24 hours duration with progressive worsening. He had been evaluated earlier at a different ED, where he received oral antihistaminic and steroid drugs without subsequent improvement. The physical examination revealed pronounced oedema in the eyelids, lips and nose (Fig. 1). Due to a strong suspicion of bradykinin-induced angio-oedema, C1 inhibitor (C1-INH) was administered through the intravenous (IV) route (twice), followed by IV aminocaproic acid and subcutaneous icatibant (twice) due to a lack of response. A review of the medical history revealed a previous diagnosis of acquired angioedema due to C1-INH deficiency following several episodes of feet swelling. In a few hours, the patient exhibited slow but progressive improvement (Fig. 2). At present, the patient is in treatment with tranexamic acid for prophylaxis and on-demand icatibant.
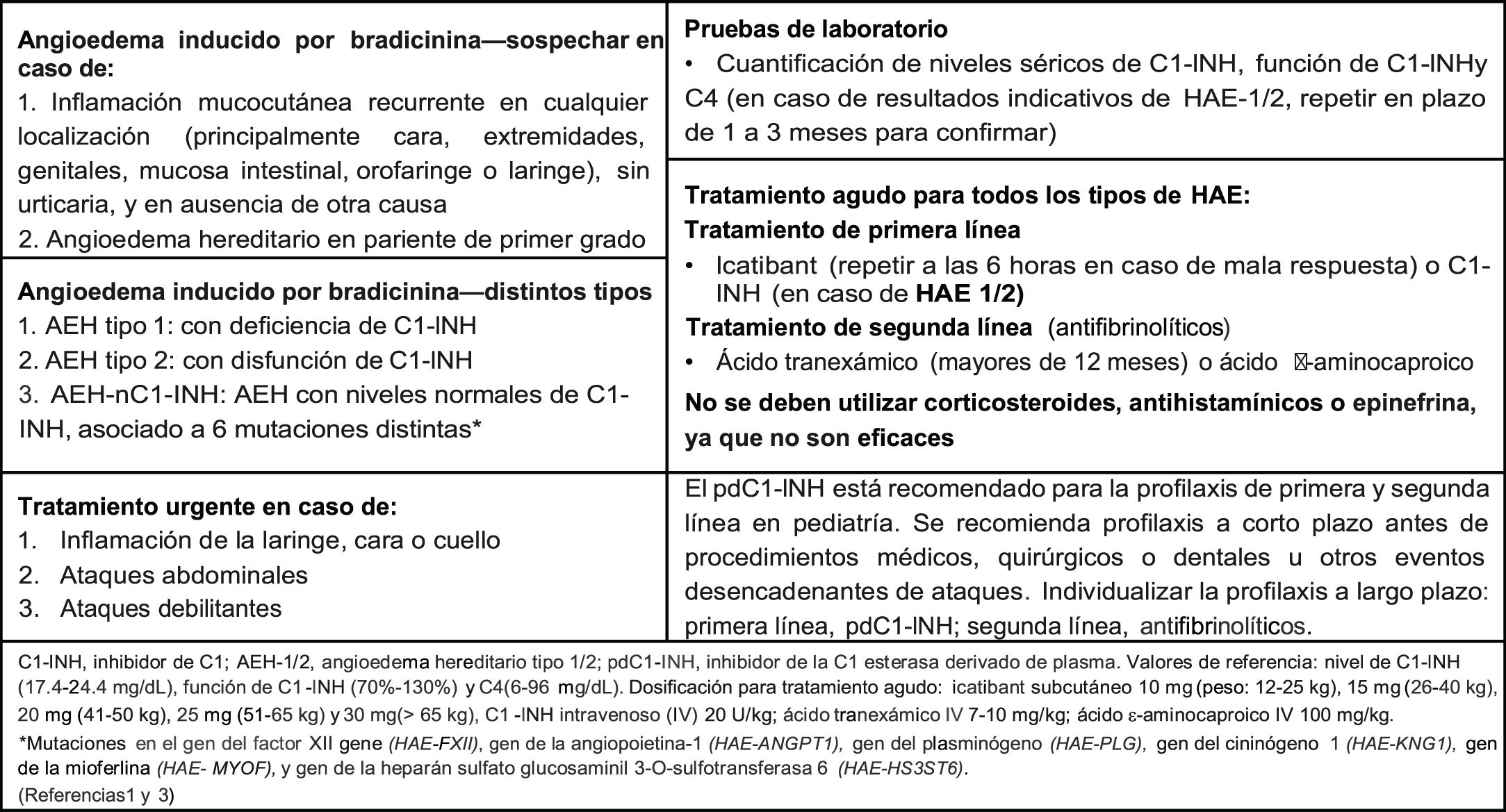
Angio-oedema and C1-INH deficiency are potentially fatal diseases characterised by oedema of the skin or mucosae involving chiefly the skin, gastrointestinal tract and upper respiratory tract.1–3 Early treatment reduces the duration of the attack, so it is crucial to identify patients who could benefit from it (Fig. 3).1–3 In the case of our patient, the delay in the initiation of appropriate treatment could explain his delayed response, which underscores the importance of the identification and treatment of angio-oedema in order to prevent the associated morbidity and mortality.
Ethical considerationsThe authors obtained the written informed consent of the legal guardians of the patient.