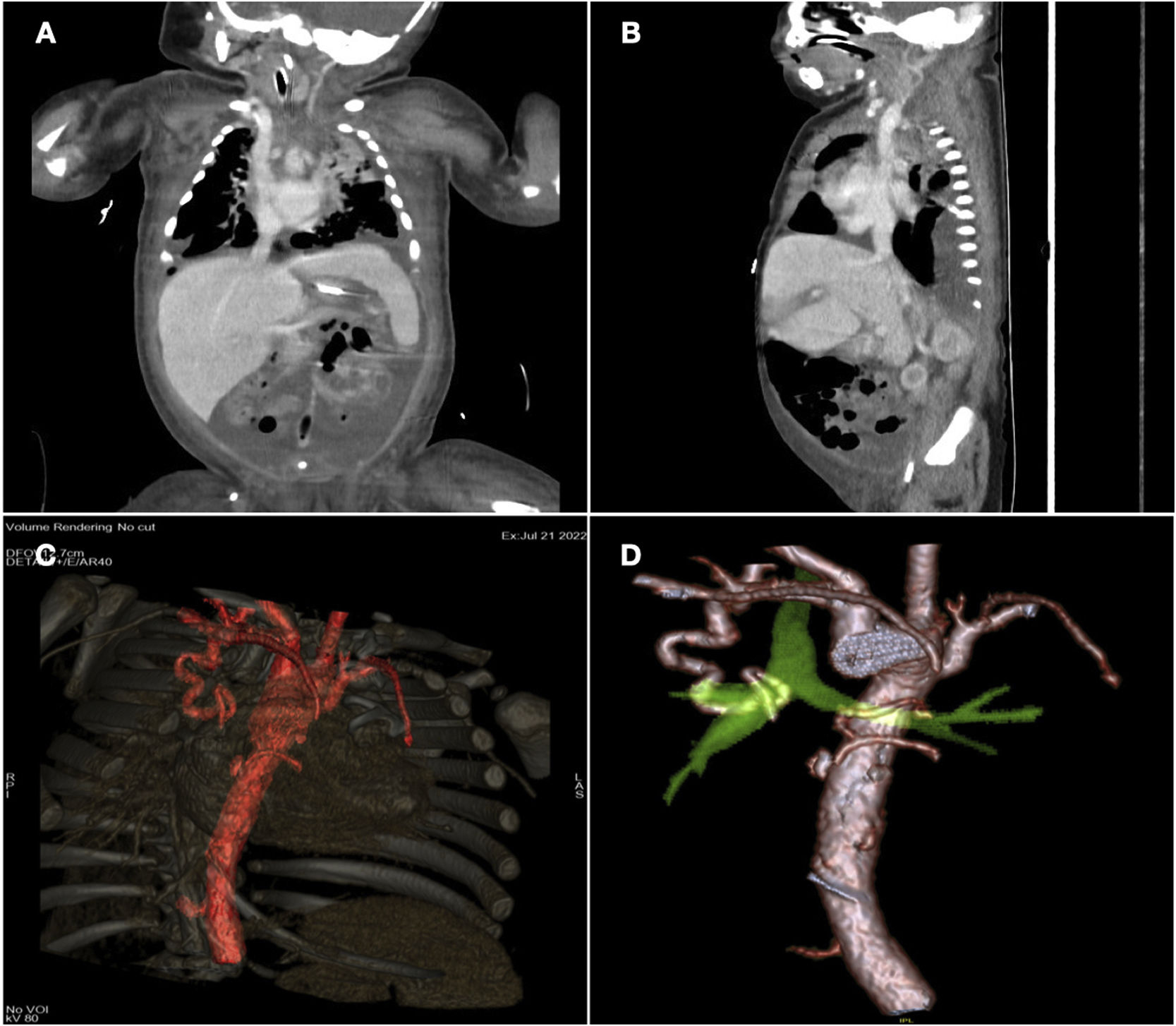
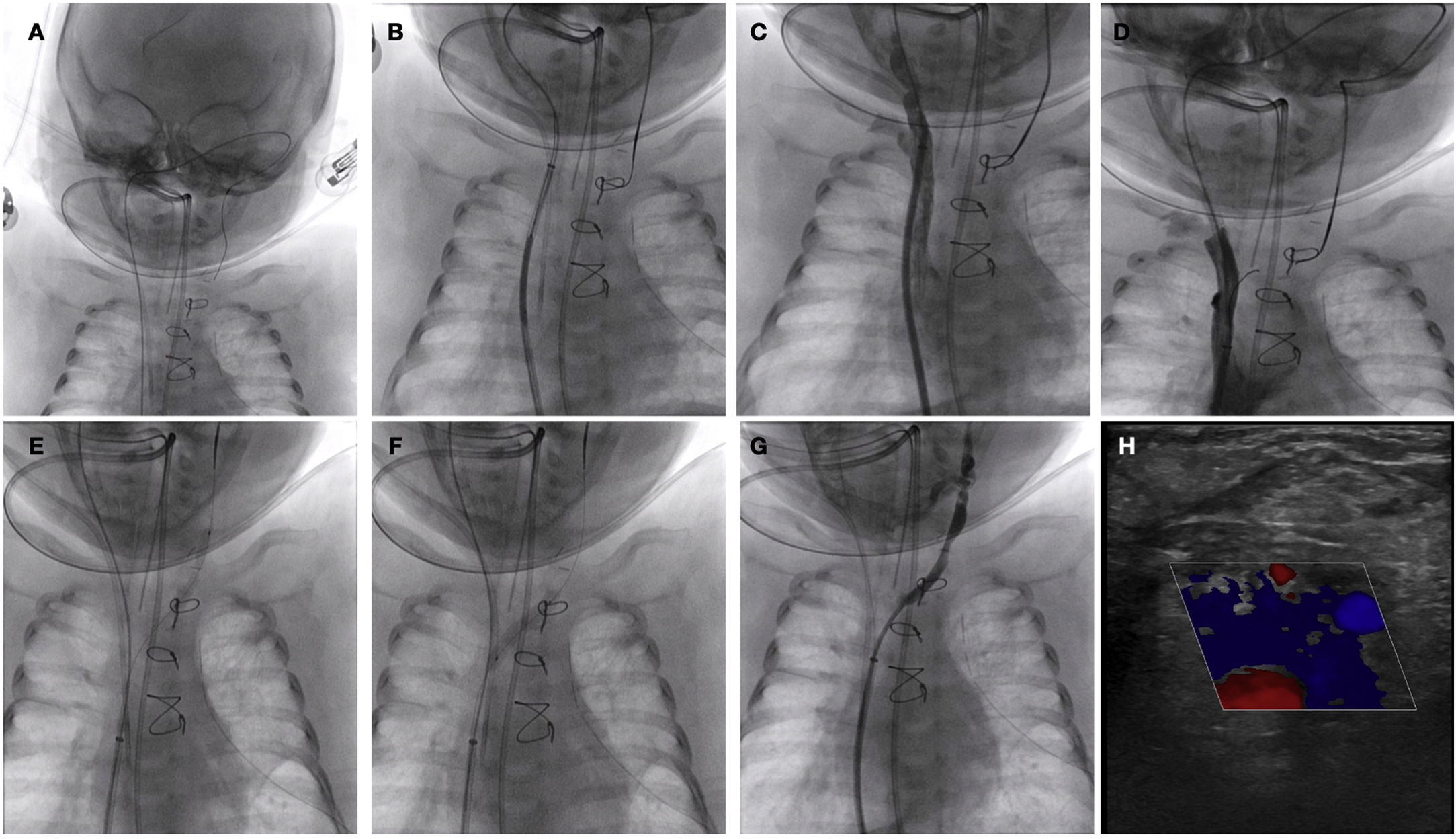
We present the case of an infant aged 2 months with dextrotransposition of the great arteries who had undergone arterial switch surgery. The patient could not be extubated due to left-side chylothorax1 and haemoptysis, with radiological evidence of occlusive thrombosis of the left jugular-subclavian venous system and an aberrant right bronchial artery2 originating from the right subclavian artery (Fig. 1). The chosen approach was percutaneous procedure in 2 steps. A dual femoral approach was used for venous recanalization, reaching the left jugular vein through the intracranial venous system, then advancing through the innominate vein to the origin of the left jugular vein, establishing a veno-venous shunt. This was followed by progressive balloon predilatation, in which the largest calibre corresponded to a Tyshak mini balloon (NuMED) measuring 6 × 20 mm, achieving recanalization of the innominate artery and the left jugular and subclavian arteries (Fig. 2; Appendix B, video 1).
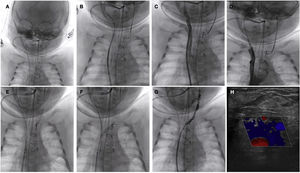
(A–C) Advance of the angioplasty guide wire and microcatheter from the right internal jugular vein through the intracranial venous system to the left jugular vein. (D) Crossing through the innominate vein to establish the veno-venous shunt. (E and F) Progressive balloon predilatation. (G) Final result with patency of the left jugular-subclavian venous system. (H) Follow-up Doppler ultrasound examination before discharge confirming the persistence of luminal patency.
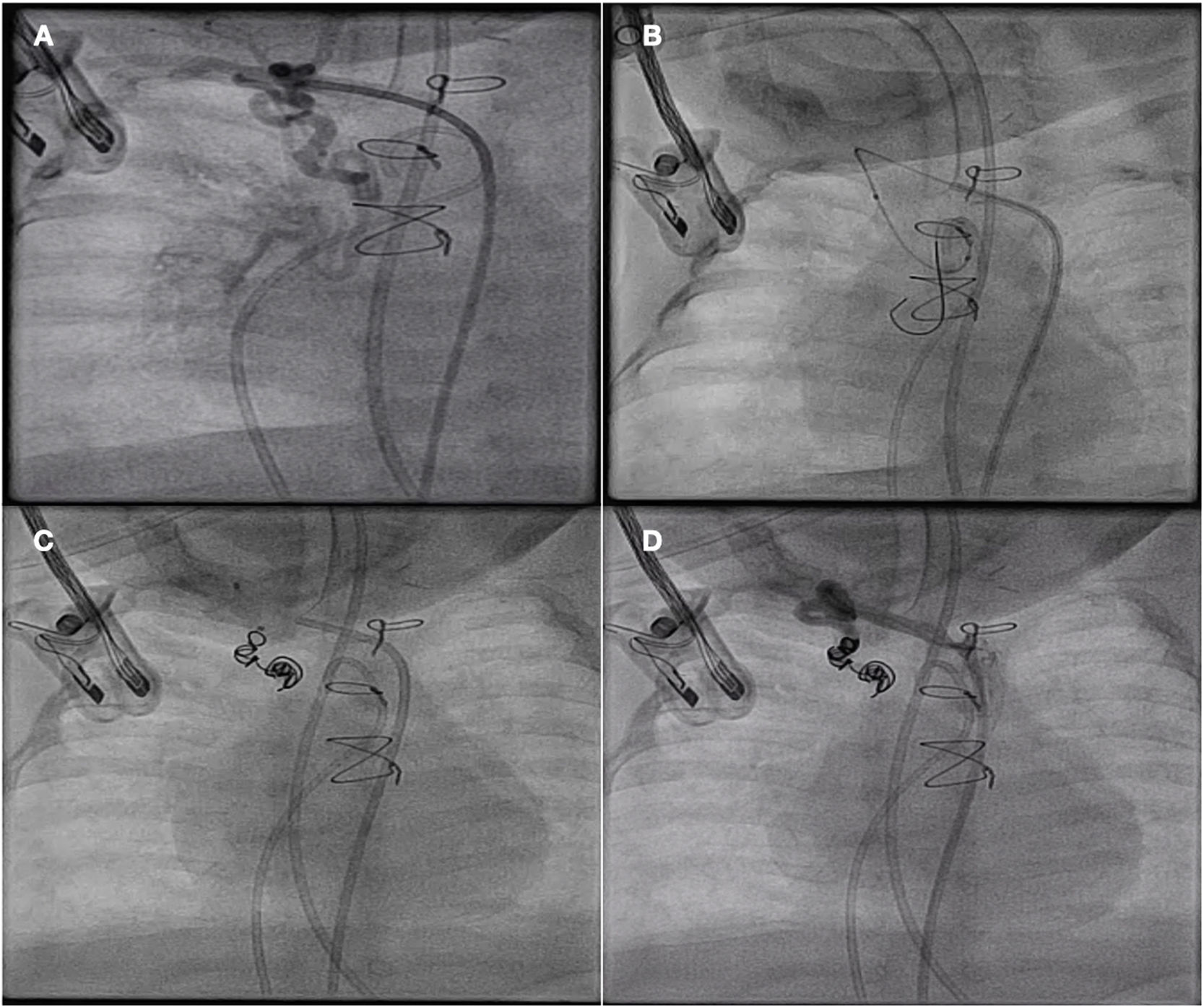
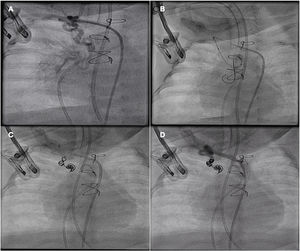
A second procedure, via arterial access, involved selective catheterization of the bronchial artery, advancing a coronary guidewire and a Cantata microcatheter (Cook medical, USA) to the medial region, where 6 microcoils were delivered, achieving full embolization (Fig. 3; Appendix B, video 2). The outcome was favourable, and the patient could be extubated and discharged from hospital.