Midline cervical cleft (MCC) is a defect in the development of the anterior region of the neck that accounts for 2% of congenital malformations of the neck,1 and some authors consider it within the spectrum of branchial arch developmental abnormalities.2 Its aetiology is unknown, and it is characterised by 4 main features: an atrophic mucosal surface, a subcutaneous fibrous cord, a caudal sinus tract and a nipple-like skin projection. Given the risk of complications, the first line of treatment is surgical excision with performance of Z-plasties to prevent anterior neck contracture, respiratory distress, micrognathia and infection and for aesthetic reasons.1
We present the cases of 4 patients operated for correction of MCC in our hospital, whose clinical and demographic characteristics can be found in Table 1. Of the 4 patients, 3 were male, and their age at the time of surgical intervention ranged from 8 to 18 months. None had a relevant personal history or associated malformations. All patients had the lesion at birth and patient 4 had undergone a biopsy of the nipple-like skin tag in a different facility at age 3 months, leading to a histological diagnosis of mixed hamartoma of the skin. In all patients, the lesions exhibited the 3 main features of MCC: an atrophic surface, a blind sinus at the inferior end, and a retractile fibrous cord (Fig. 1). Patient 1 also had a nipple-like protuberance at the superior end, as can be seen in Fig. 1. Patient 2 had a minimal nipple-like skin tag. In all patients, the lesion was more apparent on neck hyperextension, and in patient 3 it hindered the full extension of the neck. All patients underwent surgical excision of the lesion through a longitudinal incision in the neck, with removal of the tissue to the level of the infrahyoid muscles and closure by Z-plasty. In every case, histological examination revealed a fistulous tract lined by a keratinising squamous epithelium, sheathed in a double layer of epithelial cells (outer cuboidal layer and inner columnar layer) without atypical or malignant cells.
Clinical and demographic characteristics of the patients.
| Patient 1 | Patient 2 | Patient 3 | Patient 4 | |
|---|---|---|---|---|
| Sex | Male | Male | Male | Female |
| Agea | 15 | 14 | 8 | 18 |
| Personal history | No | No | No | No |
| Associated malformation | No | No | No | No |
| Atrophic surface tissue | Yes | Yes | Yes | Yes |
| Fibrous band | Yes | Yes | Yes | Yes |
| Caudal sinus | Yes | Yes | Yes | Yes |
| Nipple-like protuberance | Yes | Minimal | No | No |
| Cervical retraction | No | No | Yes | No |
| Post-surgical followupb | 1 | 1 | 7 | 10 |
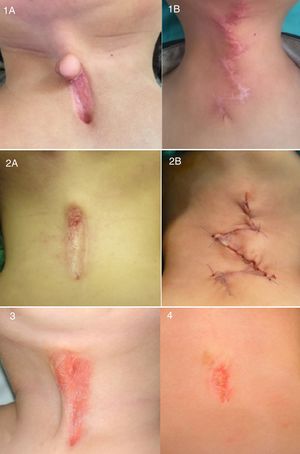
Patient 1: (A) MCC with superior nipple-like skin projection. (B) Z-plasty in case 1, 1 month post surgery, allowing cervical retraction and mobility. Patient 2: (A) MCC with very small superior nipple-like skin tag. (B) Z-plasties in case 2 after finishing surgical treatment. Patient 3: MCC hindering cervical extension. Patient 4: Small MCC manifesting with neck hyperextension.
The embryopathogenesis of MCC has not been established, although several theories have been proposed, the most widely accepted being the impaired fusion of the first or second branchial arches during the third and fourth weeks of embryonic development.1,3 Other theories include the presence of amniotic adhesions and vascular anomalies leading to tissue ischaemia, necrosis and scarring of the developing branchial arch, or increased pressure on the developing cervical area from the adjacent pericardial roof during the fifth week of gestation.2,3 However, these theories do not account for the presence of glandular tissue, cartilage, and skeletal muscle in the subcutaneous tissue.1 Midline cervical cleft usually manifests early after birth with 4 main features: an atrophic mucosal surface, a caudal sinus that may have a mucoid discharge, a fibrous cord of variable length that may extend from the lower border of the mandible to the upper border of the manubrium, which in severe cases may limit extension, as occurred in patient 3 in our study, and less frequently a nipple-like skin tag. The lesion is superficial, located in the midline, and the superficial muscles of the neck remain intact.1,2,4 It is believed that the traction of the cord on the mandibular bone during development may produce abnormalities such as exostosis, micrognathia and cleft mandible, so surgical intervention should be performed at an early stage. Midline cervical cleft may be associated with other malformations in the region, such as thyroglossal duct cyst, ectopic bronchogenic cyst, cleft tongue, lower lip and mandible or cleft sternum,2 and can also be associated with cardiac anomalies.5 The diagnosis of MCC is clinical and can be made based on the findings of physical examination, although a cervical ultrasound scan may be performed to rule out potential comorbidities. In addition, the differential diagnosis must include other diseases that are more common, such as thyroglossal or subcutaneous bronchogenic cysts of the neck.1,4 Bronchogenic cysts of the neck may be associated with MCC, as histologically they have an inner lining of ciliated pseudostratified columnar epithelium overlying a smooth muscle wall containing seromucous glands and more rarely cartilage plates, similarly to MCC.4
Treatment consists in the complete removal of the lesion with closure by means of Z-plasties, as this method avoids the formation of a vertical scar and is thus less likely to result in wound contracture, while allowing lengthening of the skin in the anterior neck.1,2
In conclusion, MCC is an infrequent disease, yet one that clinicians should be aware of on account of its potential complications. Surgical intervention should be performed early to prevent these complications, such as anterior neck contracture, respiratory distress, micrognathia and infection.
Please cite this article as: González Ruiz Y, Burgués Prades PL, Rodríguez Márquez G, Fernández Atuán RL, Siles Hinojosa A. Hendidura cervical media: una enfermedad poco frecuente. An Pediatr (Barc). 2019;90:310–312.