The paediatrics curriculum of medicine students must include knowledge and management of the problems most commonly found in children (95% of childhood diseases, which are managed in the primary care [PC] setting) in addition to complex diseases (5%–10% of child diseases, which require hospital-based care). However, in most schools of medicine in Spain, the paediatrics curriculum focuses on hospital-based care. In 2014, the Department of Paediatrics of the Universidad Complutense of Madrid hired PC paediatricians as associate professors to lecture and serve as tutors for students in the PC rotations.
We conducted a retrospective descriptive study to analyse the characteristics and outcomes of practical training in PC paediatrics and assess the perceptions of students training in the Hospital General Universitario Gregorio Marañón of Madrid by means of an anonymous questionnaire.
Medical students do the 6-to-8-week paediatrics rotation in year 5 or 6 of their training after choosing 2 fields among the different hospital-based paediatric specialities and PC. At the end of the rotation, they submit a portfolio including a written review of the rotation and a self-evaluation, and are asked to fill out a questionnaire on a voluntary basis asking about organizational and teaching aspects and offering room to write any comments and suggestions on areas that could be improved.
In the academic years spanning from 2015 to 2018, 104 medical students of the Universidad Complutense of Madrid, affiliated to the Hospital Gregorio Marañón, did a rotation in PC paediatrics. All of them submitted the written review of the rotation, of which we were able to include 81 (78%) in the analysis, and 33 (30%) filled out the anonymous questionnaire. Students gave the training a score of 9.95 ± 0.05 (Table 1) and organizational aspects a score of 10 on a scale of 10. Table 2 presents the most common comments found in the analysis of the rotation reviews. The most frequent suggestions for improvement were prolonging the PC rotation and making the PC rotation mandatory.
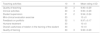
Results in the section of teaching activities of the anonymous questionnaire.
| Teaching activities | 10 | 9 | Mean rating ± SD |
|---|---|---|---|
| Quality of teaching | 30 | 3 | 9.90 ± 0.29 |
| Clinical activities | 30 | 3 | 9.90 ± 0.29 |
| Student supervision | 31 | 2 | 9.94 ± 0.24 |
| Mini-clinical evaluation exercise | 33 | 10 ± 0 | |
| Feedback on portfolio | 32 | 1 | 9.97 ± 0.17 |
| Humane treatment | 33 | 10 ± 0 | |
| Overall usefulness of rotation in the training of the student | 33 | 10 ± 0 | |
| Quality of training | 30 | 3 | 9.90 ± 0.29 |
SD, standard deviation.
Most frequent comments made by students.
| Very good/excellent/the best/one of the best rotations in the educational programme |
| Learning of fundamental aspects of paediatrics /history-taking, physical examination and management of the child |
| Training on the healthy child |
| Training on the most common childhood diseases |
| Training on communication with patients and families and physician-patient rapport. Empathy |
| Biopsychosocial perspective of disease |
| Training on health education, prevention and promotion |
| Teamwork |
| Excellent treatment of students/felt very comfortable |
| The educational needs and personal wellbeing of the student were taken into account |
| Connection of theory with everyday clinical practice |
| The role of the student was well defined. The most comprehensive and organised rotation |
| Feeling that the student had a meaningful role (as opposed to feeling useless in other rotations in which the students felt like mere observers) |
| Autonomy with supervision |
| Active participation of students |
In 1999, the American Association of Pediatrics proposed 50% of the paediatrics rotation be spent in the ambulatory care setting.1 In spite of this, training in PC paediatrics has yet to be generalised.
Several studies have assessed the outcomes of PC paediatrics rotations.2–4 These studies found that students perceived these rotations very positively, as they considered them among the most valuable in their training. Our findings are consistent with this, as students reported considerable satisfaction with both the organization and the quality of the training. Students highlighted the acquisition of knowledge and skills in the management of healthy children, the history-taking and physical examination in the assessment the most common diseases, the biopsychosocial approach to disease management, health promotion and prevention activities, communication with patients and families, teamwork, autonomy and active participation. They also praised how students were treated.
Some studies have also assessed the performance of students following the rotation,5,6 and while no difference was found in the performance of the objective structured clinical examination (OSCE),5 the assessment of the management of the most frequent complaints in the paediatric population did find differences.6 Furthermore, these studies reported that students that did a PC rotation saw 4 times as many patients that also presented with more frequent paediatric complaints compared to students that did rotations in the hospital setting.5
There are several limitations to our study. The study was performed in a single university hospital, and the response rate was relatively low, although we were able to analyse the rotation reviews submitted by a substantial percentage of the students, which we therefore believe reflect the perceptions of students accurately. In addition, our study did not allow us to determine whether higher student satisfaction correlated to better learning outcomes and translated to better care delivery in future clinical practice.
In conclusion, medical students had a very positive perception of the PC paediatrics rotation. They considered that they had learned essential aspects of the management of children, families and the most common childhood diseases in addition to non-essential technical aspects. Training in ambulatory settings complements training in the hospital setting, and both are necessary to obtain a comprehensive education in paediatrics. The rotation in PC allows students to acquire basic clinical skills while working with real-world patients, which are harder to acquire in the hospital setting, and get training in areas such as health prevention and promotion or the biopsychosocial approach to disease.
We believe that the rotation in PC paediatrics should be mandatory in the curriculum of every medical school in Spain and integrated with hospital-based rotations with specific goals. To this end, it is advisable that PC paediatricians be included in the teaching staff of university paediatrics departments. Our experience may provide a model for the development of the PC paediatrics rotation.
Please cite this article as: Aparicio Rodrigo M, Martínez González C, Garcia-Onieva Artazcoz M, Hernáez Cobeño Á, López-Herce Cid J. Descripción y evaluación de la rotación de estudiantes de Medicina por Pediatría de Atención Primaria. An Pediatr (Barc). 2021;94:413–415.