Ocular toxoplasmosis (OT) is the leading cause of posterior uveitis in immunocompetent patients. The primary infection is asymptomatic in most cases, and therefore OT is commonly diagnosed in subsequent reactivations manifesting with characteristics chorioretinal scars (white-yellow lesions with greyish edges, usually unilateral).
From a clinical standpoint, paediatric patients may present with retinochoroiditis and be asymptomatic, with blurry vision due to vitreitis or with bloodshot eyes and ocular pain, frequently associated with anterior uveitis. The pathogenesis of such reactivations remains unclear.1
The diagnosis is made based on the described clinical manifestations combined with compatible serological findings. Most patients have low IgG titres and negative IgM titres, so IgG avidity or increased titres may be useful for diagnosis.2 Challenging cases may require the use of invasive techniques, such as polymerase chain reaction (PCR) analysis for detection of Toxoplasma gondii in aqueous or vitreous humour3; however, this is considered an aggressive technique.
We present 3 cases of acquired OT in paediatric patients, describing characteristic signs that can be assessed by optical coherence tomography (OCT) and that contributed to the early and accurate diagnosis of the disease.
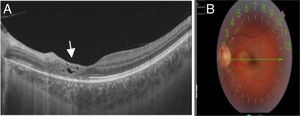
Case 1: girl aged 8 years from Equatorial Guinea that presented with acute unilateral anterior uveitis manifesting with eye pain and redness. The patient underwent immunological testing and screening for infections including serological tests for antibodies against Toxoplasma, with a negative result for IgM antibodies and a positive result for IgG antibodies. The fundus appeared normal in the initial examination. In subsequent evaluations, the patient had elevation of IgG antibodies and the OCT revealed retinitis with stalagmite-like raised lesions in the inner perimacular surface, suggestive of toxoplasmosis4 (Fig. 1).
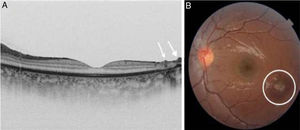
Case 2: boy age 12 years of Spanish descent presenting with headache and loss of visual acuity (0.8). Examination of the fundus revealed focal chorioretinitis focal with vitreitis, compatible with toxoplasmosis, while serological testing for antibodies against Toxoplasma was negative for IgM and positive for IgG. Subsequent evaluations revealed a 4-fold increase in IgG titres. Treatment started with antibiotherapy and systemic steroid therapy. The outcome was parafoveal scarring with absence of photoreceptors and small retinal cysts, with normal visual acuity (Fig. 2).
A) OCT image. Cystic spaces in the inner layer of the retina. Cystic spaces are a frequent finding in patients with toxoplasmosis and considered a complication (parasite-filled cysts or signs of local inflammation or exudates). B) Photograph of the eye fundus showing the paramacular chorioretinal scar in the nasal fundus, consistent with the OCT findings.
Case 3: girl aged 10 years of Moroccan descent presenting with panuveitis with acute granulomatous anterior uveitis in the left eye. The ophthalmological evaluation by means of OCT revealed areas of inflammation, signs of vitreitis and inflammation of the inner layers of the retina. Ocular toxoplasmosis was suspected, leading to serological testing, which was positive for IgG, with a titre of more than 200 U/mL, and negative for IgM. The patient started a course of antibiotherapy, to which she responded favourably. Subsequent ophthalmologic evaluations revealed an area of chorioretinal atrophy with absence of pigmentation in the margins. Visual acuity was not affected.
These 3 patients were treated with pyrimethamine-sulfadiazine and oral corticosteroids, to which they responded favourably. The clinical and serological outcomes confirmed the diagnosis of uveitis secondary to Toxoplasma infection. In OCT, focal retinitis with adjacent vitreitis is highly suggestive of OT. Newly identified clinical signs that may be found with OCT, such as early signs of inflammation (stalagmite-like lesions) (Fig. 1), or residual signs, such as retinal cysts5 (Fig. 2) are not specific for toxoplasmosis and have been described in association with other diseases (intraocular lymphoma). However, they can help guide the diagnosis of OT and prevent the use of more invasive techniques, such as PCR analysis of vitreous fluid. The presence of residual cysts could be related to the pathogenesis of infection reactivations. The establishment of a standardised protocol for assessment with OTC and further studies on the subject could increase our understanding of OT.
Please cite this article as: Ferrer Mellor T, et al. Novedades para el diagnóstico de la toxoplasmosis ocular: uso de la tomografía de coherencia óptica. An Pediatr (Barc). 2020;92:105–106.