Survival in paediatric patients with Hodgkin lymphoma (HL) has increased over the last decades. However, these patients are at increased risk of developing late thyroid sequelae due to the treatment with irradiation and alkylating agents.
MethodsWe conducted an observational and retrospective study in patients with a diagnosis of HL between 2007 and 2022, in a hospital that is a paediatric oncology reference centre, through the review of electronic health records. We collected data on demographic (age, sex), clinical, radiological and histopathological variables, the dosage of alkylating agents and radiotherapy (RT) and on thyroid disorders using Microsoft Excel. The data analysis was conducted with SPSS version 17, using the Fisher exact test for qualitative data, a nonparametric test for quantitative data and Kaplan-Meier curves.
ResultsSixty patients received a diagnosis of HL from 2007 to 2022. The median duration of follow-up was 78.5 months. There were 4 detected cases of hypothyroidism, 5 of thyroid nodules and 1 of subclinical hyperthyroidism. Treatment with RT was significantly associated with the development of hypothyroidism (P= .026), thyroid nodules (P= .01) and thyroid disease overall (P= .003). We estimated that the risk of thyroid disease increased 8-fold with each additional Grey received (hazard ratio, 1.081; 95% CI, 1.014–1.152; P= .017).
ConclusionHodgkin lymphoma patients treated with RT are at increased risk of late thyroid disorders, mainly hypothyroidism and malignancy. This risk is greater the higher the RT dosage and the longer the follow-up. We did not find evidence of an association between the use of alkylating agents and an increase in the risk of thyroid disease.
La supervivencia de pacientes con linfoma de Hodgkin (LH) se ha incrementado en las últimas décadas. Sin embargo, el tratamiento con radioterapia (RT) y alquilantes aumenta el riesgo de desarrollo de patología tiroidea a largo plazo.
MétodosSe realizó un estudio observacional y retrospectivo en un hospital de referencia para oncología pediátrica, de pacientes diagnosticados de LH desde 2007-2022 mediante revisión de historias clínicas del sistema “Historia Clínica Electrónica” (HCIS). Se recogieron en Microsoft Excel datos demográficos (edad, sexo), clínicos, radiológicos y anatomopatológicos, así como dosis de RT y alquilantes recibidas, y alteraciones tiroideas encontradas. Estos datos fueron analizados mediante el sistema estadístico SPSS17, utilizando test de Fisher para análisis cualitativo y pruebas no paramétricas para las variables cuantitativas, así como curvas de Kaplan-Meier.
ResultadosSe diagnosticaron 60 pacientes con LH, con una mediana de seguimiento de 78,5 meses. Se detectaron 4 casos de hipotiroidismo, 5 nódulos y un caso de hipertiroidismo subclínico. El tratamiento con RT resultó estadísticamente significativo para el desarrollo de hipotiroidismo (p=0,026), nódulos tiroideos (p=0,01) y patología tiroidea total (p=0,003). Este riesgo aumenta a razón de un 8% por cada grey administrado (p=0,017, HR=1,081, IC95%=1,014–1,152).
ConclusionesLos pacientes con LH tratados con RT presentan un mayor riesgo de desarrollo de patología tiroidea a largo plazo, principalmente hipotiroidismo y neoplasias. Este riesgo aumenta cuanto mayor es la dosis recibida y mayor el tiempo de seguimiento. No se ha podido demostrar que los agentes alquilantes aumenten el riesgo de desarrollo de patología tiroidea.
Hodgkin lymphoma (HL) is the most frequent type of cancer in adolescents and accounts for fewer than 5% of new cancer diagnoses in children aged less than 15 years.1 The treatment is based on combination chemotherapy regimens, restricting radiation therapy (RTX) for high-risk patients with low chemosensitivity. In recent decades, new drugs have been introduced, such as monoclonal antibodies and immune checkpoint inhibitors, chiefly used for second-line treatment in the paediatric population. At present, the cure rate is greater than 90% in patients with localised disease and no risk factor and ranges between 60% and 80% in patients with advanced disease.1
This significant increase in survival calls for the development of long-term follow-up programmes, like the one established in our hospital, which is a reference centre for paediatric oncology, to monitor the potential late adverse events of treatment, such as cardiovascular, pulmonary or musculoskeletal disease, infertility or other endocrine disorders or second neoplasms.2,3
The incidence of thyroid disorders and thyroid cancer is greater in HL survivors compared to the general population, but it is difficult to calculate objective estimates of risk for these events due to the heterogeneity and interference of the different treatments, the small sample sizes and the short duration of follow-up in previously published studies.3
The aim of our study was to describe the incidence of thyroid disorders and thyroid cancer in a retrospective cohort of children and adolescence with a diagnosis of classic HL and treated in the department of paediatric haematology and oncology of a national and international reference centre.
Material and methodsWe conducted a retrospective observational study including patients aged 0–18 years given a diagnosis of HL in our hospital (a reference centre for paediatric oncology) between 2007 and 2022 through the review of the electronic health records (HCIS database). We used Microsoft Excel® to collect data on demographic (age, sex), clinical, radiological and histological characteristics, the doses of RTX (expressed in Gy) and alkylating agents (cyclophosphamide equivalent dose [CED], calculated with the formula published by Green et al.)4 and the detected thyroid abnormalities. These data were analysed with the statistical package SPSS version 17, using the Fisher exact test and the linear-by-linear χ2 test for the analysis of qualitative data and nonparametric tests for quantitative data, in addition to generating Kaplan-Meier curves.
Thyroid abnormalitiesThe defined 5 types of thyroid abnormalities: (a) hypothyroidism: abnormal laboratory results (thyroid stimulating hormone [TSH] > 5.5 μIU/mL; thyroxine [T4] < 0.63) and clinical manifestations; (b) hyperthyroidism: abnormal laboratory results (TSH<0.36 μIU/mL, free thyroxine [fT4] > 1.4ng/dL) and clinical manifestations; (c) subclinical hypothyroidism: abnormal laboratory results (TSH>5.5 μIU/mL, fT4 and free triiodothyronine [fT3] within the normal range) in absence of compatible symptoms; (d) subclinical hyperthyroidism (TSH<0.36 μIU/mL or undetectable and fT4 and fT3 within the normal range) in absence of symptoms and (e) thyroid nodules: detected by ultrasound.
We generated contingency tables grouping the 5 abnormalities into 3 categories: hypothyroidism overall (clinical hypothyroidism+subclinical hypothyroidism), hyperthyroidism overall (clinical hyperthyroidism+subclinical hyperthyroidism) and thyroid nodules. We assessed the association of these categories with the RTX, alkylating agents and combined RTX+alkylating agents treatment variables.
Ethical considerationsThe study was designed and carried out in adherence to the International Code of Medical Ethics and the principles of the Declaration of Helsinki. Confidentiality was strictly safeguarded in the handling of personal data, conforming to the current legislation on personal data protection: Organic Law 3/2018, of 5 December, on the Protection of Personal Data and the Guarantee of Digital Rights, and Regulation (EU) 2016/679 of the European Parliament and of the Council. The data used in the study were retrieved from the health records of the patients and were identified using a numerical code and collected in a research file in the centre. The study did not require direct contact with the patients and all the data were collected retrospectively for a study period spanning 15 years, so we requested the exemption from informed consent as established in current law. The project was approved by the Ethics Committee of Research with Medicines of our hospital (file R-0089/22; 31 January 2023).
ResultsA total of 62 cases of HL were diagnosed in our hospital in the period under study. Of them, 2 were excluded because we were not able to obtain data on the treatment received by the patients. Of the 60 patients included in the analysis, 31 were male patients and 29 female, and the median age at diagnosis was 13.6 years (interquartile range [IQR], 11.5–15.6). Table 1 summarises the stages and types of HL diagnosed in the patients, the provided treatments and the detected thyroid abnormalities.
Summary of the descriptive analysis.
| Variable | n (%) |
|---|---|
| Total number of patients | 60 (100%) |
| Sex | |
| Male | 31 (51.7%) |
| Type of HL | |
| NOS | 7 (11.7%) |
| Nodular sclerosing | 45 (75%) |
| Mixed cellularity | 6 (10%) |
| Lymphocyte rich | 1 (1.7%) |
| Lymphocyte-predominant | 1 (1.7%) |
| Stage | |
| I | 1 (1.7%) |
| II | 31 (51.7%) |
| III | 12 (20%) |
| IV | 16 (26.7%) |
| Treatment | |
| First-line | 54 (90%) |
| Second-line | 3 (5%) |
| Unknown | 3 (5%) |
| Protocol | |
| SEOP-EH-01 | 1 (1.7%) |
| SEOP-EH-03 | 3 (5%) |
| EuroNet-PHL-C1 | 15 (25%) |
| EuroNet-PHL-C1 interim | 15 (25%) |
| EuroNet-PHL-C2 | 17 (28.3%) |
| EuroNet-PHL-C2 interim | 5 (8.3%) |
| Other | 4 (6.7%) |
| CTX with alkylating agent | 50 (83.3%) |
| RTX | 25 (41.7%) |
| Goitre | 1 (1.7%) |
| Laboratory and/or sonographic abnormality | 9 (15%) |
| Genetic disorder/Family Hx of thyroid disease | 2 (3.3%) |
CTX, chemotherapy; EuroNet PHL-C1, First international inter-group study for Classical Hodgkin's Lymphoma in children and adolescents; EuroNet PHL-C2, second international inter-group study for classical Hodgkin lymphoma in children and adolescents; HL, Hodgkin lymphoma; Hx, history; NOS, not otherwise specified; RTX, radiotherapy; SEOP-EH, Hodgkin lymphoma management protocol of the Sociedad Española de Oncología Pediátrica.
Of the 60 patients included in the study, 54 received first-line treatment based on the protocol that was current at the time (SEOP-EH-01, SEOP-EH-03, Euronet-PHL-C1, Euronet-PHL-C1 interim, Euronet-PHL-C2, Euronet-PHL-C2 interim) (Table 2), while 3 patients received chemotherapy and/or RTX regimens outside the protocol. Three patients were referred to our hospital for second-line treatment. In addition, 16.6% (10/60) of the patients experienced recurrence during follow-up in our hospital and required second-line treatment. Of these patients, 70% (7/10) underwent autologous peripheral blood stem cell transplantation (PBSCT). In the overall sample, 3 of the 60 patients (5%) died during the follow-up: one due to infectious complications during first-line treatment, one due to infectious complications during pretransplant conditioning and the last one after the PBSCT.
Chemotherapy regimens.
| Protocol | Treatment group | Chemotherapy | Alkylating agents |
|---|---|---|---|
| SEOP-EH-01 | OPPA+COPP | Cyclophosphamide, procarbazine | |
| SEOP-EH-03 | OPPA/OEPA+COPP | Cyclophosphamide, procarbazine | |
| EuroNet PHL-C1 | TG-1 | OEPA | 0 |
| EuroNet PHL-C1 | TG-2 | OEPA+COPP/COPDAC | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C1 | TG-3 | OEPA+COPDAC±ABVD | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C1 Interim | TG-1 | OEPA | 0 |
| EuroNet PHL-C1 Interim | TG-2, TG-3 | COPDAC±OEPA | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C2 | TL-1 | COPDAC+OEPA | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C2 | TL-2 | DECOPDAC+OEPA | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C2 | TL-3 | COPDAC+OEPA | Cyclophosphamide, dacarbazine |
| EuroNet PHL-C2 Interim | TL-1, TL-2 | COPDAC/DECOPDAC+OEPA±GEV±bendamustine | Cyclophosphamide, dacarbazine |
| Other | ABVD/DHAP/BEACOPP/IGEV | Cyclophosphamide (BEACOPP) | |
| BEAM | Melphalan |
ABVD: doxorubicin (Adriamycin), bleomycin, vinblastine, etoposide, prednisone, cyclophosphamide; BEACOPP: bleomycin, etoposide, doxorubicin, cyclophosphamide, vincristine, prednisone and procarbazine hydrochloride; BEAM: carmustine, cytarabine, melphalan, etoposide; COPDAC: cyclophosphamide, vincristine, prednisone and dacarbazine; COPP: cyclophosphamide, vincristine, procarbazine and prednisone; DECOPDAC: doxorubicin, etoposide, cyclophosphamide, vincristine, prednisone, dacarbazine; DHAP: dexamethasone, cisplatin, cytarabine; EuroNet PHL-C1: First international inter-group study for Classical Hodgkin's Lymphoma in children and adolescents; EuroNet PHL-C2: second international inter-group study for classical Hodgkin lymphoma in children and adolescents; IGEV: ifosfamide, gemcitabine, vinorelbine; OEPA: vincristine, prednisone, etoposide, doxorubicin (Adriamycin); OPPA: vincristine, prednisone, procarbazine, doxorubicin (Adriamycin); SEOP-EH: Hodgkin lymphoma management protocol of the Sociedad Española de Oncología Pediátrica; TG: treatment group; TL: treatment level.
Eighty-three percent (50/60) of the patients was treated with alkylating agents, and the median CED was 4971mg/m2 (IQR, 3685.5–7452.94mg/m2). In the overall sample, 41.6% (25/60) of patients received RTX for the head and neck with a median dose of 25Gy (IQR, 19.8−29.8Gy), and 35% (21/60) were treated with alkylating agents as well as RTX (Tables 1 and 3).
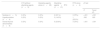
Median administered doses.
| Treatment | Total | With thyroid abnormalities | Without thyroid abnormalities | P |
|---|---|---|---|---|
| Radiotherapy (Gy) | 25.0 (19.8−29.8) | 29.8 (19.8−29.8) | 20.0 (19.8−29.8) | .577 |
| Dose: median (IQR) | ||||
| Alkylating agent (mg/m2) | 4971 (3685.5−7452.94) | 5771 (3299.81−15 824.72) | 4378.25 (3685.5−7616.81) | .763 |
| Dose: median (IQR) |
IQR, interquartile range.
After a median of 78.5 months of follow-up (IQR, 42.5–113.75), thyroid abnormalities were identified in 16.7% of the patients: 3.3% developed hypothyroidism, 3.3% subclinical hypothyroidism, 1.7% subclinical hyperthyroidism and 8.3% thyroid nodules, of which 4/5 were malignant (papillary thyroid cancer). Only one of the patients with a thyroid nodule also had subclinical hypothyroidism.
Of the 50 patients who received alkylating agents, 12% (6/50) developed thyroid abnormalities having received a median dose of 5771mg/m2 (IQR, 3299.81–5824.72mg/m2). Patients without thyroid disorders received a median of 4378.25mg/m2 (IQR, 3685.5−7616.81mg/m2), without statistically significant differences between these two groups (P=.763) (Table 3).
Of the 25 patients who received RTX, 32% (8/25) developed thyroid abnormalities, having received a median dose of 29.8Gy (IQR, 19.8−29.8Gy). The median RTX dose in patients without thyroid abnormalities was 20Gy (IQR, 19.8−29.8Gy) (Table 3). There were no significant differences in the development of thyroid disorders based on the RTX dose (P=.577).
We performed an exploratory analysis of the observed frequency of thyroid complications based on the received treatment (alkylating agents, RTX or alkylating agents+RTX) and found no significant differences in frequency. Then, we categorised the received treatments in 4 groups ordered by the frequency of thyroid-related events obtained in the previous analysis. The groups were ordered from lower to higher frequency: other treatments (neither RTX nor alkylating agents), alkylating agents alone, alkylating agents+RTX and RTX alone. Table 4 presents the results. To obtain more homogeneous results in this analysis, we excluded the single case of hyperthyroidism.
Trends in the frequency of thyroid disorders based on the received treatment. The single case of hyperthyroidism was excluded.
| CTX without alkylating agents (n=6) | Alkylating agents alone (n=28) | Alkylating agents+RTX (n=21) | RTX alone (n=4) | χ2 test | ||
|---|---|---|---|---|---|---|
| P | Trend (P) | |||||
| Nodules (n=5) | 0 (0%) | 0 (0%) | 2 (9.5 %) | 3 (75%) | <.001 | <.001 |
| Hypothyroidism (n=4) | 0 (0%) | 0 (0%) | 3 (14.3%) | 1 (25.0%) | .092 | .020 |
| Overall thyroid abnormalities (n=8) | 0 (0%) | 0 (0%) | 5 (23.8%) | 3 (75%) | <.001 | <.001 |
Total patients included: 59.
CTX, chemotherapy; RTX, radiotherapy.
As can be seen in Table 4, we found a significant association for presence of thyroid nodules and the presence of thyroid abnormalities overall (P<.001), but not for hypothyroidism. These findings show that the use of RTX alone increases the probability of thyroid complications to a greater extent compared to the use of alkylating agents, alone or even combined with RTX.
In the multivariate analysis, RTX was a risk factor for the development of thyroid abnormalities, and the risk increased with the duration of follow-up (P=.028; hazard ration [HR], 10.246; 95% confidence interval [CI], 1.279–82.056). We estimated that each Gy increase in the administered dose corresponded to an 8% increase in risk (P= .017; HR, 1.081; 95% CI, 1.014–1.152) (Fig. 1).
Lastly, we found no statistically significant differences in the development of thyroid cancer based on sex (P=.792) or the age at treatment initiation (P= .191).
DiscussionIn recent decades, advances in both the diagnosis and treatment of HL have contributed to an increase in survival rates. Along with this increase in survival, there has been evidence of a substantial number of long-term sequelae that has generated a growing interest in the development of optimal follow-up strategies.5,6 It is important to keep in mind that thyroid complications, both in the form of functional impairment and neoplasms, can manifest even decades later and are usually have indolent and nonspecific clinical manifestations.7,8
HypothyroidismIn our study, the overall frequency of thyroid abnormalities (laboratory and sonographic) was 16.7%. Of these abnormalities, 6.7% corresponded to cases of hypothyroidism (clinical or subclinical). Hypothyroidism is the thyroid complication described most frequently in survivors of childhood HL.9 Some studies have found frequencies of up to 60%, depending on the population under study and the criteria used to define hypothyroidism.5 The proportion of cases in our study, which is considerably lower, was probably due to the small sample size compared to most other studies and the shorter duration of follow-up.
We found a statistically significant association between the use of RTX and the development of hypothyroidism. Neck irradiation is the main risk factor for the development of hypothyroidism in oncological patients, and in most studies the disorder tends to appear in approximately 30% of cases within 10 years of completing RTX.5 However, the risk of radiation-induced hypothyroidism continues to be high even 25 years after exposure to radiation.10 Furthermore, there is evidence that the risk of developing hypothyroidism after RTX is dose-dependent.9 Although we did not find statistically significant differences in the RTX dose between the group that did not develop thyroid abnormalities and the group that did, the impact of the use of RTX in the development of thyroid complications was strong and sizeable. Taking into account the small sample size in our study, the fact that these associations were statistically significant corroborates the role of RTX as a cause of thyroid damage. The median radiation dose received by patients with thyroid abnormalities was 29.8Gy. A study conducted by Sklar et al. found a prevalence of hypothyroidism of 30% associated to doses of 30–45Gy and of up to 50% for doses greater than 45Gy. In addition, in the latter group, the risk of developing hypothyroidism within 20 years of diagnosis was 50%.4 Duarte et al. found that radiation doses greater than 35Gy had a significant impact (P<.01) on the development of hypothyroidism. The findings of this study also suggested that the risk was greater in patients treated with neck and craniospinal irradiation compared to total body irradiation,11 in opposition to the study of Madanat et al., who did not find differences based on the irradiation field.12 There is also evidence of the benefits of hyperfractionated RTX compared to conventional RTX and the use of protons instead of photons to minimise the exit dose and thus the damage beyond the target tissues.8 Other risk factors associated with the development of hypothyroidism secondary to RTX are the age of exposure, dose of RTX, duration of exposure and time elapsed since the completion of treatment.8,10
The association between the use of alkylating agents and the development of hypothyroidism was not statistically significant in our study (P=.528). Few studies support this association. One of them, a report of the Childhood Cancer Survivor Study, attributed 9.4% of the total cases of hypothyroidism to the use of bleomycin and alkylating agents (cyclophosphamide and lomustine).10 However, there is controversy in regard to the potential causative role of CTX and, for the time being, there are little data that support it.5,13
Thyroid nodulesOf the 5 nodules detected in our case series, 4 were diagnosed as papillary thyroid cancer after the fine-needle aspiration and biopsy. As occurred in relation to hypothyroidism, RTX was a risk factor for the development of thyroid neoplasms, benign or malignant. In paediatric patient it is even more damaging, as children aged 5–10 years are more susceptible to the noxious effects of radiation.14–16 Thyroid cancer, especially the papillary form, is one of the most frequently diagnosed second neoplasms in survivors of childhood cancer.17 Broadly speaking, the time elapsed from the diagnosis of the primary cancer and the development of secondary neoplasms varies widely in the literature,18 as they can develop within 4 years of treatment completion6 or even 20 years after.17 And while the increase in risk declines gradually over time, the risk never becomes as low as the risk in the general population.19
In our case series we found a statistically significant association between the use of RTX and the development of thyroid nodules (P= .01). It has been described that any increment in the dose of radiation increases the risk of second thyroid cancer,8 although there seems to be a downturn in the dose-response relationship from approximately 20Gy. This suggests that the greater the radiation dose the thyroid parenchyma is exposed to, the greater the direct cell-killing effect and therefore the fewer viable thyrocytes that remain to undergo malignant transformation.8,20,21 However, in our study, the median RTX dose in the group of patients who developed thyroid cancer was 29.8Gy.
When it came to age and sex in relation to the development of thyroid neoplasms, we did not find any significant differences. However, a study conducted in HL survivors with second thyroid cancer found that patients irradiated at younger ages and female patients were at increased risk.22 The multivariate analysis of a more recent study found that age less than 20 years (P= .032) and female sex (P= .016) were associated with a greater probability of second cancer.11 The disagreement of our results with the overall trends reported in the literature is very likely due to the limitations imposed by the small sample size and the short duration of follow-up.
The role of alkylating agents in the development of neoplasms, as occurred with hypothyroidism, is not well established. A report from the Childhood Cancer Survivor Study shows that 119 cases of thyroid cancer were identified in a cohort of 12 547 patients with a median duration of follow-up of 5 years. There was a statistically significant association between the detection of thyroid cancer and combined treatment with RTX (at a dose < 20Gy) and alkylating agents (relative risk [RR], 4.7; 95% CI, 1.5–15; P=.04). 23 Of the 5 patients with thyroid nodules in our case series, all received RTX and 3 did not receive chemotherapy with alkylating agents. Given the small size of the groups in the sample (5 patients with nodules and 8 with thyroid abnormalities of any kind), we were not able to assess causality in the association between the development of thyroid cancer and the use of alkylating agents.
Due to the small number of patients with papillary thyroid cancer in the case series, we could not assess the association between this disease and laboratory abnormalities.
HyperthyroidismOnly one case of hyperthyroidism (subclinical) was detected, corresponding to a frequency of 1.7% (clinical hyperthyroidism+subclinical hyperthyroidism) in our patients. Of all the possible thyroid complications, hyperthyroidism is the least frequent5 and is usually subclinical. In addition, it may be a transient complication due to a certain level of thyrotoxicosis resulting from the direct destruction of parenchyma by RTX that eventually resolves (euthyroidism).8 For this reason, assessment of thyroid function is recommended, at least a few months after RTX has been completed to avoid biased results due to the thyroiditis susceptible period that follows irradiation.11
Thyroid disorders overallWhen it came to the development of thyroid abnormalities overall, we found a strong association between the use of RTX and these abnormalities (P= .003). The multivariate analysis also found a significant association (P= .028), and, while the 95% CI was broad (1.279–82.056) due to the dispersion of the few data that we had available, the identified association suggested consistency. In addition to demonstrating this association based on the presence or absence of a history of RTX, we also estimated that for each additional Gy of radiation, the risk of developing thyroid disease increased by 8% (P= .017; HR, 1.081; 95% CI, 1.014–1.152). These findings were consistent with those of other authors such as Steven et al., who calculated an increase of 1.06 in the relative risk of hypothyroidism with each additional Gy administered (P= .000001).
Long-term follow-up and screeningGiven all that has been discussed this far, we ought to highlight the importance of close monitoring and follow-up in these patients. The number of HL survivors continues to grow, and the broad variety of sequelae and involvement at different levels require strategies with a multidisciplinary approach.24 The findings of our study and the existing literature suggest that the risk of thyroid abnormalities in survivors of childhood HL increases consistently with time. The cumulative incidence of thyroid cancer continues to grow even 30 years after the diagnosis of the primary cancer,25 and, while these radiation-induced second cancers do not appear to be more aggressive than sporadic cancers, it is important to provide adequate screening and follow-up.26 Endocrinology societies propose routine ultrasound screening in patients with a history of RTX 5, while others argue that palpation and the physical examination are sufficient and reduce the associated costs and the potential psychological distress that may be associated with a diagnostic procedure.8 Close long-term follow-up of HL survivors is necessary to detect life-threatening thyroid changes in a timely manner.
The main limitations of the study are its small sample size and its retrospective design. The duration of follow-up, short in comparison with other studies, is another limitation.
ConclusionWe found a nonnegligible frequency of thyroid disorders in the sample of survivors of HL. The most frequent thyroid complications were hypothyroidism and thyroid neoplasms.
There is evidence that RTX can cause thyroid disease, and the risk of its development is dose-dependent and increases with time.
We found no conclusive evidence that the use of alkylating agents, alone or combined with RTX, increased the risk of thyroid disorders. Additional studies in larger samples would be needed to prove whether such an association exists.
Conflicts of interestThe authors have no conflicts of interest to declare.
I would like to express my appreciation for the interest, attention and dedication of all the authors that have participated in the development of the manuscript, with particular emphasis on the work of Dr Paloma Conejero González, the educational guidance of Dr Maitane Andión and the statistical analysis of Alberto Martín Vega.