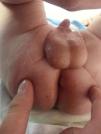
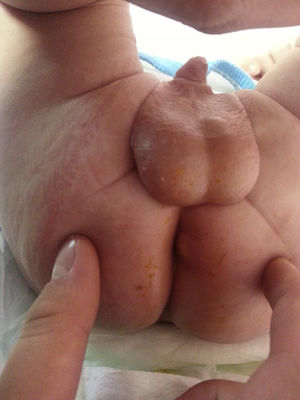
There are limited data on the aetiology and management of perianal abscesses (PAs). The aim of this retrospective study was to define the characteristics of children with PAs; describe our experience with PA from the perspective of paediatric infectious medicine and determine the factors that influence clinical outcomes.
MethodsWe performed a retrospective review of cases of PA in children with no underlying disease managed in a tertiary referral hospital between January 2005 and July 2015. We collected data on demographic characteristics, symptoms, abscess size and location, abscess recurrences, laboratory and microbiological findings, treatment modalities, diagnosis of systemic illness at the end of the diagnostic workup and clinical outcomes.
ResultsWe included a total of 47 patients in the study, with a predominance of male patients (93.6 vs 6.4%, P<.001). The median age was 7.7 months (IQR 1.8–13.7 months), and 40 children (85.1%) were younger than 2 years of age. Four PAs drained spontaneously and 7 healed without need of drainage (23.4%). Drainage by simple incision was applied to 36 patients (76.5%) and six PAs required fistulotomy (12.7%). Recurrent abscesses were found in 25 patients (53.1%). Three patients with recurrent PA were diagnosed with inflammatory bowel disease at the end of the diagnostic evaluation.
ConclusionsBased on the findings of our study, measurement of white blood cell counts and serum levels of acute phase reactants may be useful in the initial evaluation of children with PA. In light of the high relapse rates observed in surgically managed patients, it seems reasonable to use a conservative approach in patients aged less than 2 years.
Existen datos limitados acerca de los abscesos perianales (AP), con respecto a su etiología y tratamiento. Este estudio retrospectivo tiene como objetivo definir las características de los niños con AP, detallar nuestra experiencia en el campo de las enfermedades infecciosas pediátricas y determinar los factores que influyen en los resultados clínicos.
MétodosEntre enero de 2005 y julio de 2015 se llevó a cabo una revisión retrospectiva de niños con AP sin enfermedad subyacente en un hospital de referencia de nivel terciario. La información incluyó características demográficas, síntomas, tamaño y localización del absceso, recurrencias de los abscesos, hallazgos de laboratorio y microbiológicos, modalidades de tratamiento, diagnóstico de enfermedades sistémicas al finalizar las investigaciones etiológicas y pronóstico.
ResultadosEn el estudio se incluyeron 47 pacientes, con predominio masculino (93,6 frente a 6,4%, p<0,001). La mediana de edad fue de 7,7 meses (rango intercuartílico 1,8 a 13,7 meses) y 40 de los niños (85,1%) tenían menos de 2 años de edad. Cuatro AP drenaron espontáneamente y 7 curaron sin necesidad de drenaje (23,4%). Se aplicó drenaje mediante incisión simple a 36 pacientes (76,5%) y 6 AP requirieron de fistulotomía (12,7%). Se observaron abscesos recurrentes en 25 pacientes (53,1%). Tres pacientes con AP recurrentes fueron diagnosticados de enfermedad inflamatoria intestinal al finalizar las investigaciones.
ConclusionesDe acuerdo con los hallazgos del presente estudio, la determinación de la cifra de leucocitos, así como de los reactantes de fase aguda, parece ser útil en la primera evaluación de los niños con AP. En cuanto a las altas tasas de recurrencia en pacientes sometidos a procedimientos quirúrgicos, resulta razonable el uso de enfoques conservadores para pacientes menores de 2 años.
Perianal abscesses (PAs) are soft tissue infections of the perianal region of unknown aetiology, although some authors have proposed an association with congenital abnormalities of the crypts of Morgagni. It has been suggested that deeper crypts may lead to the trapping of debris and cryptitis. The organisms isolated most frequently from PAs are a mix of aerobic and anaerobic flora. Systemic symptoms are rare and most abscesses drain spontaneously, which is what has given rise to the debate as to the evaluation and management of PAs.1 Most patients with PA are male, and more than 50% of cases develop in infants younger than two years of age.2 In older patients, the aetiology shifts to underlying diseases such as inflammatory bowel disease (IBD), leukaemia or immunocompromised states.3
There is a dearth of data on the aetiology, management, and underlying diseases associated with PAs, particularly in children. Many of these data are from studies on the surgical treatment of PAs and its different modalities published by surgeons.2–6 Therefore, we aimed to define the characteristics of children with PAs, describe our experience with PA as specialists in paediatric infectious diseases, and identify factors that influence clinical outcomes.
Material and methodsWe conducted a retrospective study by reviewing the outpatient and inpatient health records of children with PA managed in our Department of Paediatric Infectious Diseases. The selected study period was January 2005 to July 2015. We collected data on the following: clinical and demographic characteristics; medical history; symptoms including fever, irritability, size, and location of abscess; recurrence status; laboratory findings including complete blood count, serum levels of C-reactive protein (CRP) erythrocyte sedimentation rate (ESR) and blood chemistry tests; initial immunological work-up including immunoglobulin tests, lymphocyte subsets, and nitroblue tetrazolium (NBT) blood test; typing and antimicrobial susceptibility of microorganisms isolated from pus cultures; need for hospital admission and length of hospital stay; dose, duration, side effects, and results of antimicrobial treatment; need and type of surgery (surgical drainage including incision and drainage, fistulotomy); diagnosis of systemic illness at the end of diagnostic workup; and clinical outcome.
We established abscess sizes based on the recorded diameters, which were estimated by the paediatric surgeons. The location of abscesses was mapped with the patient in the prone position and described using the numbers that occupy the same position on a clock face. Recurrence was defined as an abscess developing more than once in the same location. An event of recurrence stated in the history of patient at the time of first admission to our center and the recurrence observed in our follow-up were included in the analysis.
White blood cell (WBC) and platelet counts, serum CRP levels (normal range, 0–0.5mg/dL), the ESR (normal range, 0–20mm/h), and blood chemistry parameters were recorded at baseline and during treatment. We retrieved data from patient reports, health records and electronic administrative and laboratory databases. We excluded patients with a previous history of PA developed in the context of systemic disease. The study was approved by the local board of ethics.
Statistical analysisWe analyse the data with the software IBM SPSS Statistics for Windows, version 22.0 (IBM Corp; Armonk, NY, USA). We summarised participant baseline characteristics with descriptive statistics, including mean, standard deviation (SD), median and interquartile range (IQR) for continuous variables, and frequency distributions for categorical variables. We used the χ2 test or Fisher's exact test to compare baseline values for the categorical variables. The normality of the distribution of quantitative variables was assessed by means of the Shapiro–Wilk test. We compared continuous by means of the t test for independent samples if the normality assumption was met and otherwise with the nonparametric Mann–Whitney U test. We defined statistical significance as a P-value of less than 0.05 in any of the tests (two-tailed).
ResultsBetween January 2005 and July 2015, a total of 29015 patients were managed in our outpatient clinics, and all of them underwent screening. Forty-seven patients (161/100000) with PAs and without underlying disease were eventually included in the study, 44 male (93.6%) and 3 female (6.4%) (P=.001). The median age in the sample was 7.7 months (IQR, 1.8–13.7 months). Forty patients (85.1%) were aged less than 2 years. Among the cases of PA for which records were available, 21.2% had presented with fever and 21.2% with irritability at the time of admission (Table 1).
Characteristics of patients with perianal abscess.
| Variable | Patients (n=47, %) |
|---|---|
| Age (months)a | 7.7 (1.8–13.7) |
| Age groupsb | |
| <24 months | 40 (85.1) |
| ≥24 months | 7 (14.8) |
| Sex (male) | 44 (93.6) |
| Symptoms at admissionb | |
| Fever | 10 (21.2) |
| Irritability | 10 (21.2) |
| Recurrenceb | |
| No surgical intervention (n=11) | 6 (54.5) |
| Any type of surgical intervention (n=36) | 19 (52.7) |
| Laboratory resultsa | |
| WBC count (/mm3) (n=41) | 11000 (8100–13600) |
| CRP (mg/dL) (n=33) | 0.17 (0–0.3) |
| ESR (mm/h) (n=24) | 2 (0–12) |
| Treatment approachb | |
| No drainage | 7 (1.8) |
| Drained spontaneously | 4 (8.5) |
| Simple incision and drainage (I/D) | 36 (76.5) |
| Fistulotomy* | 6 (12.7) |
| Antibiotics** | |
| No antibiotics | 2 (4.2) |
| β lactam/β lactamase inhibitor | 24 (51) |
| Other combinations | 21 (44.6) |
Out of the 25 records for which there was documentation about the site of the abscess, the most common localizations were 9 o’clock, in 14 cases (28%), and 3 o’clock, in 7 (14%), followed in decreasing frequency by 2, 11, and 8 o’clock (Fig. 1). Out of the 25 cases in which the abscess size was documented, the size was less than 2cm in 16 (64%) and larger than 2cm in 9 nine (36%).
The median total WBC count was 11000mm−3 (IQR, 8100–13600) (Table 1). Three patients (6%) that presented with neutropenia at admission (absolute neutrophil count <1500mm−3) had recovered by six months of followup and did not receive a definitive diagnosis. Three patients (6%) had low immunoglobulin levels for age, which improved throughout the followup. None of the patients in the sample had low NBT results. In our sample, CRP values had been recorded for 33 patients, and were within the normal range in 25 (75.7%), with a median CRP level of 0.17mg/dL (IQR, 0–0.3). The median ESR for the sample was 2mm/h (IQR, 0–12), while six patients (25%) had ESRs of more than 20mm/h (Table 1).
We found records for the results of pus cultures of 34 patients. There was no growth in the cultures corresponding to 13 of the patients. As for the pus cultures where growth was detected, Escherichia coli (E. coli) was the only isolated organism in 10 (29%), a mix of enteric flora (E. coli, Klebsiella spp, Proteus spp was detected in 18 (52%), and the growth was considered indicative of contamination by skin flora in the remaining 3 (8.8%). Treatment included antibiotherapy in all patients but 2, with a combination of at least two classes of antibiotics in 96% of those that received them (n=45); the combination prescribed most frequently consisted of beta-lactam agents/beta-lactamase inhibitors plus ornidazole (n=24; 51%).
Four PAs drained spontaneously and 7 healed without need of drainage (23%). Drainage by simple incision was used in 76% of patients (n=36), and 6 of the abscesses required fistulotomy (12.7%). Fifty-three percent of the patients (n=25) had recurrent abscesses. Of the patients whose PAs drained spontaneously or healed without drainage, 6 (40%) had recurrent abscesses, and the rate of recurrence in patients treated with any type of surgical intervention was 52% (Table 1).
Three patients with recurrent PA and elevation of ESR and CRP received diagnoses of IBD (1 of ulcerative colitis and 2 of Crohn's disease) at the end of the evaluation. One was a child aged less than 2 years of age that received a diagnosis of infantile Crohn's disease, and the other two were aged more than 2 years. Table 2 presents the demographic and laboratory characteristics of these patients.
Characteristics of patients with a final diagnosis of IBD.
| Patient 1 | Patient 2 | Patient 3 | |
|---|---|---|---|
| Final diagnosis | Ulcerative colitis | Crohn's disease | Crohn's disease |
| Age | 104 months | 15 months | 43 months |
| Sex | Male | Male | Male |
| WBC (/mm3) | 10900 | 5400 | 12800 |
| ESR (mm/h) | 72 | 120 | 66 |
| CRP (mg/dL) | 4.8 | 24 | 6.2 |
| Surgical treatment | Incision/drainage | Incision/drainage+fistulotomy | None |
| Recurrence | Yes | Yes | Yes |
| Abscess location | 9 o’clock | 9 o’clock | 9 o’clock |
We grouped and analysed patients based on the presence of recurrent abscess. Patients who had elevated WBC counts at admission were significantly less likely to have a recurrent PA (P=.006). On the other hand, sex, age, presence of fever or irritability, abscess size, abscess location and the modality of surgical treatment did not differ significantly between the recurrent PA and non-recurrent PA groups. When we compared patients aged less than 24 months and older patients, we found that the presence of fever at admission was significantly less frequent in patients aged less than 2 years (P=.009). The WBC count and ESR were also significantly higher in the younger group compared to the group of patients aged 24 or more months (P=.016 and P=.001, respectively).
DiscussionBased on the findings of our study, a WBC count, levels of acute phase reactants and a gastrointestinal evaluation may be useful in the initial evaluation of children with PA.
We analysed data for a total of 47 children with a diagnosis of PA, and an underlying cause—ulcerative colitis, Crohn's disease or neutropenia—was found in 6 of the total (12.8%). As could be seen in our study, approximately 10% of anorectal abscesses may have aetiologies other than anal gland infection, such as Crohn's disease, trauma, immunodeficiency, neutropenia, malignancy, tuberculosis, hidradenitis suppurativa, foreign bodies, inflammatory bowel disease, dermal cysts and radiotherapy.3 It has been reported that 4% of paediatric patients with Crohn's disease may present with perirectal or perianal lesions without a site of primary intestinal disease. Ulcerative colitis is also occasionally associated with perianal lesions.7,8 Three of the patients in our study that presented with no known disease or symptoms other than PA eventually received a diagnosis of inflammatory bowel disease. These patients had recurrent abscesses and high ESR and CRP values, which suggest the presence of chronic inflammation. We hypothesise that measurement of the ESR and CRP levels may help us identify an ongoing process of chronic inflammation in the absence of other indicative manifestations in patients with recurrent abscesses. Three other patients who were healthy prior to the development of PAs had neutropenia at the time of admission, which had resolved by six months of followup in the outpatient clinic. Since the aetiological investigation of the neutropenia did not identify any diseases, we believe that the neutropenia observed at the time admission may have been a transient manifestation of a viral infection. None of the patients received a diagnosis of primary immunodeficiency. Thus, we concluded that a complete blood count and a peripheral blood smear are necessary tests in the evaluation of PA, especially in recurrent cases.
Chronic granulomatous disease (CGD) should be included in the differential diagnosis of perianal abscess in infants. Winkelstein et al. reported that at least one PA was found in 15% to 18% of CGD patients,9 but none of our patients received a diagnosis of CGD or any other immunodeficiency disease. Therefore, additional immunological tests, such as the NBT test, quantification of immunoglobulin levels or lymphocyte subsets probably need not be routinely included in the initial evaluation of well-appearing children with PA. We suggest restricting testing for immunodeficiency diseases to patients that present with recurrent PAs in association with other symptoms.
Over 90% of the patients in our sample were male, which was consistent with other studies.4,5 It has been hypothesised that this difference between sexes may be due to an excess of androgen in cases of androgen–oestrogen imbalance, or to the abnormal development of androgen-sensitive glands in utero.9
Perianal abscesses are a simple and quite common condition that occurs mostly in infants.10 In our study, 85% of patients were infants. They are most prevalent in paediatric patients, with an estimated incidence of 0.5–4.3%. Probably due to its low incidence, there are few studies of PA in children aged more than 2 years, except for studies of cases with underlying disease. The pathogenesis of PA in infants has yet to be elucidated. Perianal abscess is defined as a local collection of pus in perianal tissues, and it is believed that the aetiology frequently involves the infection of glands in the anal crypts.11 The most common organisms isolated from perianal abscesses are mixed aerobic bacteria (E. coli, Klebsiella pneumonia, Staphylococcus aureus) and anaerobic bacteria (Bacteroides spp., Clostridium).12 In our study, 52% of the cultures yielded mixed aerobic species, while E. coli was the only isolated pathogen in 29% of patients.
The vast majority of anorectal abscesses develop spontaneously in completely healthy children and have a self-limiting course. In contrast to PAs in the adult population, the paediatric forms are rarely associated with systemic manifestations of sepsis.13 In our study, over 50% of the patients had no fever or discomfort at the time of admission, corroborating the benign presentation of PAs in most patients. In the patients for whom records of the abscess size and location were available, abscesses were mostly small (<2cm) and located at 9 o’clock and 3 o’clock, findings that were similar to those of previous studies.2
The conservative management of PAs continues to be subject to debate. In our study, 38% of pus cultures showed no growth, and patients were treated with antibiotics, mostly with combinations consisting of a beta-lactam/beta-lactamase inhibitor plus ornidazole. In addition, 4 abscesses drained spontaneously, 7 healed without drainage, and only 6 required fistulotomy. Based on the data published by Christison-Lagay et al., nonoperative management with hygiene measures, sitz baths and antibiotherapy is an appropriate approach to the treatment of PA in infants.14 Furthermore, Serour et al. reported that the incidence of fistulas was lower in patients who treated locally with or without antibiotics compared to patients that underwent drainage.4 Based on a study conducted on a limited number of patients, Rosen et al. concluded that some surgical procedures, including fistulotomy or fistulectomy, may be unnecessary, and that antibiotherapy also appears to be of limited use.13 In addition to this evidence, studies have also been conducted to assess the effectiveness of traditional remedies in the nonoperative management of PA. One study found that treatment with hainosankyuto treatment (TJ-122) was more effective than incision and drainage in the management of PA in infants.15 The rates of recurrence of perianal abscess and/or development of a fistula-in-ano after treatment of PA reported in the literature range between 6% and 85%.12,16–19 Consistent with this, the recurrence rate in our study was 53.2%. Although our results were not statistically significant, the recurrence in patients that underwent any type of surgical intervention was similar to that in patients that healed without surgery. Thus, in light of the high relapse rate found in our patients and reported in other studies,12,16–19 we share the opinion that conservative management is justifiable, especially in patients aged less than 2 years. In addition, we compared relapsing and non-relapsing PAs based on the WBC count and found that PA recurred less frequently in patients with high WBC counts (P=.006). One possible explanation is that a stronger initial immune response prevents recurrence of PA.
To our knowledge, this is one of the few studies analysing the association between age, clinical manifestations and first-line laboratory test results in children with PA. The proportion of patients that presented without fever was significantly greater in the group aged less than 2 (P=.009). The WBC count and ESR were also significantly higher in the same group compared to the group aged 2 or more years (P=.016 and P=.001, respectively). As regards general practitioners, it would be reasonable to state that in the initial step of the evaluation, infants are more likely to present without fever and with higher levels of acute phase reactants.
We ought to mention some of the limitations of our study. First of all, the sample was relatively small, and we obtained the data from a retrospective review of health records, so we were unable to collect all the relevant information in detail. Therefore, our results need to be confirmed in a larger, randomised prospective trial. Secondly, there was no standardised approach to management guiding the selection of antimicrobial treatment (type, duration, or combination of several antimicrobials) or surgical intervention. Therefore, we are unable to reflect on the most appropriate surgical approaches or antimicrobial regimens. Nevertheless, we believe that our results are highly relevant due to the scarcity of studies focused on the underlying conditions of children with PA from a paediatric infectious disease perspective, as opposed to a surgical perspective, which is the usual focus of published studies.
In conclusion, we aimed to summarise our data on PAs in children without underlying disease at admission from a paediatric infectious disease perspective. We have highlighted the evaluation of chronic inflammatory processes in children with PAs that are recurrent or present with elevated acute phase reactants. We recommend conservative management in children aged less than 2 years to allow the possibility of spontaneous resolution.
Conflict of interestsThe authors declare that they have no conflicts of interest.
Please cite this article as: Tanır Basaranoglu S, Ozsurekci Y, Cengiz AB, Karadag Oncel E, Aykac K, Kara A, et al. Absceso perianal en niños: perspectiva desde el campo de la infectología pediátrica. An Pediatr (Barc). 2019;90:370–375.