Paroxysmal supraventricular tachycardia (PSVT) is the most frequent form of sustained tachycardia in childhood. It is defined as tachycardia caused by a rhythm disorder originating above the His bundle.
Its most frequent electrocardiographic presentation is regular tachycardia with a narrow QRS complex. The heart rate is usually greater than 180–220 beats per minute (bpm) in infants, and at least 120–150 bpm in older children. It responds to vagal manoeuvres and drugs that slow conduction through the atrioventricular node. Clinically, it is well tolerated, but when it is prolonged, patients may develop signs of congestive heart failure.1
The main goal of acute treatment is to stop the arrhythmia, slow down the ventricular response and restoring the sinus rhythm. In stable patients, the initial management should consist of vagal manoeuvres, as they can succeed in ending the tachycardia in cases involving the atrioventricular node in the conduction pathway. In school-aged children and adolescents, this is mainly achieved through the Valsalva manoeuvre, as both ocular pressure and carotid sinus massage are not recommended in these age groups.2 In paediatric patients, the effectiveness of vagal manoeuvres ranges between 30% and 60%.3,4
One of the ways to increase the vagal parasympathetic tone is to increase venous return. Studies in adults have investigated different modifications of the traditional Valsalva manoeuvre technique to increase vagal tone. In particular, the study conducted by Appelboam et al.5 found a statistically significant increase in the effectiveness of nonpharmacological measures with the performance of the so-called modified Valsalva manoeuvre, increasing the cardioversion success rate by a factor of 2.5, with a 28% reduction in adenosine administration. In the paediatric population, there is the additional advantage that patients tend to respond better to vagal manoeuvres (30%–60% of children compared to 17% of adults).
To date, no studies have been published analysing the effectiveness of this manoeuvre in the paediatric population.
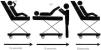
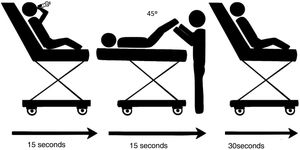
We conducted a multicentre prospective study with data collection between February 2019 and January 2021. Before its initiation, the study received the approval of the competent ethics committee. The sample consisted of cooperative children aged 6 or more years with a diagnosis of PSVT who were haemodynamically stable. After explaining the procedure and obtaining the signed informed consent, the patient underwent the modified Valsalva manoeuvre, as shown in Fig. 1: starting with the patient standing, the patient exhales forcefully into a 10 mm syringe against the resistance of the plunger for 15 s. Then, the patient is placed in the supine position with the lower extremities elevated for 15 s, and finally stands again for 30 s.
We collected data for the 8 patients with PSVT treated with the modified Valsalva manoeuvre. Three were male and 5 female, and their median age was 9.5 years. All but one had had previous episodes. Of these 7, 3 had needed adenosine to control the tachycardia, and 2 patients received daily treatment with atenolol.
In 6 of the 8 patients (75%) the modified Valsalva manoeuvre was effective, in 4 in the first attempt (50%). The modified manoeuvre succeeded in restoring the sinus rhythm in 2 out of the 3 patients who had needed adenosine in the past.
As for the 2 patients who ultimately needed adenosine, one received antiarrhythmic treatment at home, and in the other, the manoeuvre had initially achieved cardioversion, but the tachycardia recurred in a few minutes.
All patients remained stable and had favourable outcomes, and none experienced adverse events following the performance of the manoeuvres.
Table 1 summarises the characteristics of the sample.
Characteristics and outcomes of patients with PSVT who underwent the modified Valsalva manoeuvre.
| Age (years) | Sex | Previous episodes | Treatment of previous episodes | Current treatment | Time elapsed from onset (minutes) | Heart rate (bpm) | Number of attempts of Valsalva manoeuvre | Administered antiarrhythmic drugs |
|---|---|---|---|---|---|---|---|---|
| 9 | Female | Yes | Spontaneous resolution | No | 15 | 260 | 2 | Not needed |
| 12 | Female | No | – | No | 180 | 183 | 1 | Not needed |
| 7 | Male | Yes | Traditional Valsalva | No | 120 | 212 | 2 | Adenosine |
| 10 | Female | Yes | Adenosine | Clorazepate dipotassium | 20 | 240 | 3 | Not needed |
| 6 | Female | Yes | Adenosine | Atenolol | 60 | 180 | 1 | Not needed |
| 10 | Male | Yes | Spontaneous resolution | No | 20 | 200 | 1 | Not needed |
| 13 | Female | Yes | Traditional Valsalva | No | 60 | 190 | 1 | Not needed |
| 9 | Male | Yes | Adenosine | Atenolol | 60 | 221 | 3 | Adenosine |
In adults, there is evidence that the modified Valsalva manoeuvre is safer and more effective in reverting PSVT. In addition, this is a modification of the traditional manoeuvres that is simple and non-invasive. In our experience, the performance of this modified manoeuvre in haemodynamically stable cooperative paediatric patients achieved very satisfactory outcomes in terms of safety and successful cardioversion, although the sample was small. Further studies are required to establish firm indications for the use of the modified Valsalva manoeuvre in the paediatric age group.
FundingThe study did not receive any specific financial support from agencies in the public, private or non-for-profit sectors.
Red de Investigación de la Sociedad Española de Urgencias de Pediatría (RISeuP-SPERG).
Noa Ramos Gómez (illustrator).