Infection by novel coronavirus (severe acute respiratory syndrome coronavirus 2, SARS-CoV-2), first identified in 2019 in Wuhan, China, is the aetiological agent of the coronavirus disease 2019 (COVID-19).1 At present, it has spread to become a global pandemic that, according to the World Health Organization, affects more than one and a half million people throughout the world.2 When the COVID-19 outbreak was first described, there were only exceptional cases in the paediatric population, but as the outbreak spread the number of reported cases in children has grown, with most affected patients having mild or no symptoms.3
The most frequent manifestations include fever, dry cough, sore throat, headache, asthenia, myalgia and respiratory distress. To date, cutaneous manifestations in association with COVID-19 have only been described in adults.3,4 Given the scarce information on these symptoms in the paediatric population, we present the cases of 2 paediatric patients with infection by SARS-CoV-2 with cutaneous manifestations.
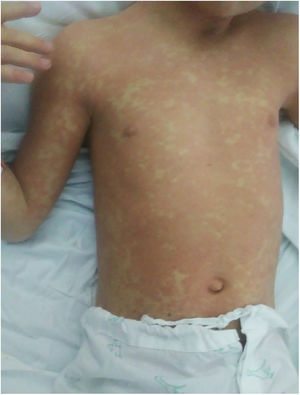
The first case corresponded to a boy aged 6 years admitted to hospital for evaluation of cholestatic liver disease of unknown aetiology. At 2 weeks, after the patient developed a low-grade fever and a worsening of the markers for cholestasis and cytolytic hepatitis, he was tested for SARS-CoV-2 and turned out positive. Forty-eight hours later, the patient developed an erythematous, confluent, nonpruritic maculopapular rash with onset in the trunk and neck that gradually spread to the cheeks and upper and lower extremities, reaching the palms of the hands (Fig. 1). The cutaneous manifestations lasted a total of 5 days and resolved with no complications and without specific treatment. Improvement in the rash was associated with improvement in laboratory markers (bilirubin, transaminases and coagulation parameters). In light of the worsening of liver disease associated with the positive PCR result for SARS-CoV-2 in a nasopharyngeal swab sample, we performed a PCR test on a liver biopsy sample obtained in the initial evaluation of the patient, which was negative. During hospitalization, the patient did not exhibit any other manifestations related to infection by coronavirus.
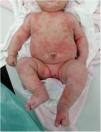
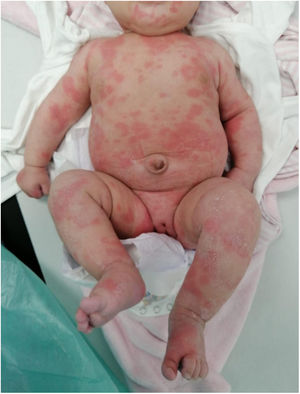
The second case corresponded to a girl aged 2 months brought to the emergency department due to a low-grade fever and acute urticaria, apparently pruritic, of 4 days’ duration. The rash was initially located in the face and upper extremities and spread in a few hours to the trunk and lower extremities (Fig. 2). The palms and soles were not affected. The patient had no angioedema in the fingers, toes, lips or tongue.
The most relevant epidemiological feature of the history was cohabitation with 2 individuals with confirmed COVID-19, which prompted performance of a SARS-CoV-2 PCR test on a nasopharyngeal swab sample that turned out positive. The patient received oral symptomatic treatment with a favorable response. Most lesions healed within 24h, and the cutaneous manifestations resolved in 5 days in the absence of any other signs and symptoms.
In the adult population, cutaneous manifestations in the context of COVID-19 have been described in a case series of 18 adult patients in Lombardy, Italy. These patients presented with nonpruritic rashes that were erythematous, urticaria-like or, in 1 case, a vesicular varicella-like rash.4 Another case was reported in Thailand in a patient with petechial exanthem that, on account of its characteristics, was initially misdiagnosed as dengue fever.5
Based on the evidence published to date,3,4 the cutaneous manifestations of novel coronavirus are similar to those caused by other common viral infections. There is no evidence that the extent of cutaneous involvement is related to the severity of disease.4 We ought to consider that in addition to the exanthems characteristic of the acute phase of infection described in this article, there have been recent reports of acral and/or chilblain-like lesions in children and youth who are otherwise asymptomatic that could be a late manifestation of inflammatory processes or microthrombotic events in the immune phase of disease.6
Contrary to what we observed in our patients, all described adult patients with cutaneous manifestations also had respiratory symptoms during the course of disease and could have received treatment for them. Thus, we also need to consider the possibility of cutaneous manifestations being adverse drug reactions.
Our observations reveal that it is possible for paediatric patients with COVID-19 to present with a rash that may be attributed to other common childhood diseases as the only manifestation or in association with mild symptoms. Given the current circumstances and the measures that have been instituted to prevent transmission in patients with suspected or confirmed COVID-19, it is particularly important to be aware of these manifestations as part of the clinical picture of the disease.
Please cite this article as: Morey-Olivé M, Espiau M, Mercadal-Hally M, Lera-Carballo E, García-Patos V. Manifestaciones cutáneas en contexto del brote actual de enfermedad por coronavirus 2019. An Pediatr (Barc). 2020;92:377–378.