In October 2008, the Valencian Community started its human papillomavirus (HPV) vaccination schedules for 14 year-old girls. The aim of this study is to assess knowledge about HPV infection and its vaccine among the mothers of these girls, and to identify factors associated with the willingness to vaccinate their daughters.
Materials and methodsCross-sectional study by means of a questionnaire to mothers of girls born in 1995, and attending secondary schools in the province of Valencia during 2010–2011. Cluster stratified random sample (n=1279). Statistical analysis: percentages, confidence intervals, OR, Chi-squared and multivariate logistic regression contrasts.
ResultsA total of 833 (65.1%) questionnaires were completed. The results obtained showed that, 76.6% of mothers had vaccinated their daughters against HPV; 93.8% knew about the vaccine, particularly through television (71.5%); and 78.5% received positive advice from a health professional which increased the vaccination of their daughters (OR: 2.4). There was low overall knowledge about HPV infection and vaccination. Confidence of the mothers in vaccines as a preventative method increases the HPV vaccination (OR: 3.8). The first reason for refusal was the fear of adverse events (45.6%).
ConclusionsApparently, the media does not influence the willingness to vaccinate. It would be desirable to minimise the perception of risk of the vaccine. Positive health advice from a health professional can have a positive effect on vaccination. There is a gap between the level of knowledge and decision-making to vaccinate.
La Comunidad Valenciana inició en octubre del 2008 el programa de vacunación contra el virus del papiloma humano (VPH) en niñas de 14 años. El objetivo de este estudio es evaluar los conocimientos sobre la infección por VPH y su vacuna en madres de adolescentes e identificar los factores asociados a la predisposición de vacunar a sus hijas.
Material y métodosEstudio observacional transversal mediante cuestionario dirigido a madres de alumnas nacidas en 1995 matriculadas en centros de secundaria de la provincia de Valencia durante 2010-2011. Muestra aleatoria estratificada por conglomerados (n=1.279). Análisis estadístico: porcentajes, intervalos de confianza, OR, contrastes chi al cuadrado y regresión logística multivariante.
ResultadosOchocientos treinta y tres cuestionarios completados (65,1%). El 76,6% de las madres habían vacunado a sus hijas contra el VPH. El 93,8% conocía la vacuna, sobre todo a través de la televisión (71,5%). El 78,5% recibió consejo favorable de un profesional sanitario, lo que mejoró la vacunación de sus hijas (OR: 2,4). Los conocimientos globales sobre la infección por VPH y la vacuna fueron bajos. La confianza de las madres en las vacunas como método preventivo mejora la vacunación contra VPH (OR: 3,8). El miedo a los efectos adversos (45,6%) fue el primer motivo de rechazo.
ConclusionesNo parece que los medios de comunicación influyan en la decisión de vacunar. Sería conveniente minimizar la percepción de riesgo ante esta vacuna. El consejo del profesional sanitario actúa a favor de la vacunación si este interviene activamente en sentido positivo. Existe una brecha entre nivel de conocimientos y toma de decisión para vacunar.
The vaccine against human papillomavirus (HPV) is administered to young adolescents to prevent potential diseases from developing in future decades, especially cervical cancer.1 There is evidence that the attitude of parents is key in achieving a high acceptability of the vaccine.2
In Spain, the Consejo Interterritorial de Salud (Interterritorial Council of Health) has recommended the inclusion of this vaccine in the routine schedule for preadolescents aged 11–14 years.3 The Autonomous Community of Valencia introduced vaccination of girls 14 years of age in 2008 with a 3-dose series. When the second dose was given to this initial cohort (first trimester of 2009) two cases of adverse events were registered following administration of the vaccine.4,5 Following two months of investigation by a group of experts, the Agencia Española del Medicamento y Productos Sanitarios (Spanish Agency of Medicines and Health Products) and the European Medicines Agency concluded that there was no causal relationship between the administration of the vaccine and the observed adverse events.4,5 These events were subject to extensive media coverage,6,7 which may have had a negative impact on the acceptability of this vaccine.8 The immediate effect was a noticeable decrease in the vaccine coverage (12%) of the second cohort compared to the first.5 Subsequent cohorts (fourth, fifth and sixth) have recovered from this decline and reached coverage rates above 70%.
The aim of this study, which was conducted after the aforementioned events, was to assess the knowledge about HPV infection and the HPV vaccine and the willingness to vaccinate the adolescent daughters of mothers residing in the province of Valencia.
MethodsWe conducted an observational, cross-sectional study for which we designed an ad hoc questionnaire to assess the prevalence of vaccination. The study was approved by the ethics and research committee of the Centro Superior de Investigación en Salud Pública (Superior Centre for Research in Publich Health) of the Health Department of the Autonomous Community of Valencia.
The target population were the mothers of girls enrolled in secondary schools in the province of Valencia during the 2010–2011 academic year. The schools were selected randomly after stratifying by type of school ownership (private, charter and public schools) and geographical location (urban, semi-urban and rural schools), obtaining a total of 31 schools.
Mothers were selected by random cluster stratified sampling. We included mothers of adolescent girls that met the official criteria for administration of the tetravalent HPV vaccine and belonged to the 1995 birth cohort. We excluded mothers that did not consent to their daughters’ participation in the study and mothers whose daughters chose not to participate.
The mothers completed a self-administered questionnaire between September 2010 and May 2011. The questionnaire had several sections: sociodemographic characteristics; personal perception of vaccination as a method of prevention; and assessment of 10 concerns, including sexually transmitted diseases (STDs), by means of a worry scale the answers to which were later dichotomised into “it worries me moderately or a lot” and “it worries me a little or not at all”.
When it came to knowledge of HPV, the questionnaire asked whether the respondent had heard of the infection and what diseases it could cause. Based on the answers, we created a new dichotomous variable to summarise knowledge of HPV. We coded having heard of the disease and answering 80% of the questions about the diseases it can cause correctly as a high level of knowledge. Participants were also asked about the sources of their information about HPV and whether they believed they were at risk of having an HPV infection.
As for the HPV vaccine, the questionnaire asked whether the respondent had heard of it and what number of doses are required for correct vaccination. Based on this data, we constructed a dichotomous variable to summarise maternal knowledge of the vaccine.
We gathered information on the type of health professional (family physician, gynaecologist, paediatrician or paediatric nurse) had informed the mother about the vaccine. We also asked whether their daughters had completed the recommended 3-dose series, and we compared the answers with the vaccination registry of the Autonomous Community of Valencia. Mothers that had not had their daughters vaccinated were asked about the main reason for not vaccinating, and who had made the decision not to vaccinate.
Statistical analysisThe dependent variable in our study was daughter vaccination status, and the remaining variables were considered explanatory variables. We have summarised the results by means of percentages and 95% confidence intervals (95% CI) for all variables under study, both for the entire sample and for the vaccinated and unvaccinated groups. To assess potential associations with vaccination, we calculated the odds ratio (OR) with its corresponding 95% CI, setting the category corresponding to the lowest proportion of vaccinated girls as the reference group. We assessed differences in the distribution of the explanatory variables and the dependent variable by means of the chi square test, considering differences statistically significant for P values of .05 or less; for measures of association (OR) we considered the results statistically significant if the 95% CI did not include 1. Subsequently, we fitted a predictive model of daughter vaccination status by multivariate logistic regression. The only explanatory variables used in the fitting of the logistic model were those that had statistically significant unadjusted ORs. Variables were introduced in the model applying the stepwise criterion. We did all the calculations with the SPSS 15.0® software.
ResultsWe originally distributed 1279 questionnaires, and received 833 back, achieving a response rate of 65.1%. The respondents were 195 (23.4%) mothers of unvaccinated girls and 638 (76.6%) mothers of vaccinated girls.
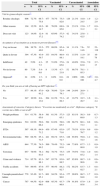
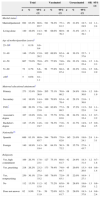
Table 1 shows the sociodemographic characteristics of the mothers and the association of those characteristics with vaccination status. Of all respondents, 83.2% were married or in a domestic partnership, and this marital status was associated with a higher vaccination coverage compared to the daughters of mothers that lived alone (OR, 1.6: 95% CI, 1.1–2.4). In the age distribution, we found only one mother aged between 25 and 30 years that we proceeded to exclude from further analyses. Of the 146 mothers aged 31–40 years (17.6%), 69.9% had their daughters vaccinated; and compared to them, mothers aged 41–50 years (73%) showed a greater willingness to vaccinate against HPV (OR, 1.5; 95% CI, 1.0–2.3) with the percentage of vaccinated daughters rising to 77.9%. We also found an association between maternal educational attainment and vaccination; mothers that had completed secondary vocational education (Formación Profesional) constituted 16.9% of the sample and 82.8% had had their daughters vaccinated, a higher frequency than the one found in mothers that had completed noncompulsory secondary education (Bachillerato), which was 70.9% (OR, 2.0; 95% CI, 1.1–3.4). Mothers of Spanish nationality (83.1%) also showed greater adherence, with 79.0% having had their daughters vaccinated compared to 64.3% of mothers of foreign nationalities (OR, 2.8; 95% CI, 1.4–3.1). We found no significant differences based on religiosity.
Description of demographic variables by vaccination status. Frequencies, percentages, 95% confidence intervals and bivariate logistic regression odds ratios.
| Total | Vaccinated | Unvaccinated | OR | 95% CI | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | |||
| Marital status* | |||||||||||
| Married/partnered | 692 | 83.2% | 80.6–85.7 | 541 | 78.2% | 75.1–81.3 | 151 | 21.8% | 18.7–24.9 | 1.6 | 1.1–2.4 |
| Living alone | 140 | 16.8% | 14.3–19.4 | 96 | 68.6% | 60.9–76.3 | 44 | 31.4% | 23.7–39.1 | 1 | |
| Age of mother/guardian (years)* | |||||||||||
| 25–30a | 1 | 0.1% | 0.0–0.4 | ||||||||
| 31–40 | 146 | 17.6% | 15.0–20.2 | 102 | 69.9% | 62.4–77.3 | 44 | 30.1% | 22.7–37.6 | 1 | |
| 41–50 | 607 | 73.0% | 70.0–76.1 | 473 | 77.9% | 74.6–81.2 | 134 | 22.1% | 18.8–25.4 | 1.5 | 1.0–2.3 |
| 51–60 | 72 | 8.7% | 6.8–10.6 | 56 | 77.8% | 68.2–87.4 | 16 | 22.2% | 12.6–31.8 | 1.5 | 0.8–2.9 |
| +60a | 5 | 0.6% | 0.1–1.1 | ||||||||
| Maternal educational attainment* | |||||||||||
| Primary | 273 | 32.8% | 29.6–36.0 | 205 | 75.1% | 70.0–80.2 | 68 | 24.9% | 19.8–30.0 | 1.2 | 0.8–1.9 |
| Secondary | 141 | 16.9% | 14.4–19.5 | 100 | 70.9% | 63.4–78.4 | 41 | 29.1% | 21.6–36.6 | 1 | |
| SVE* | 169 | 20.3% | 17.6–23.0 | 140 | 82.8% | 77.2–88.5 | 29 | 17.2% | 11.5–22.8 | 2.0 | 1.1–3.4 |
| Associate's degree | 107 | 12.8% | 10.6–15.1 | 81 | 75.7% | 67.6–83.8 | 26 | 24.3% | 16.2–32.4 | 1.3 | 0.7–2.2 |
| Bachelor's degree | 143 | 17.2% | 14.6–19.7 | 112 | 78.3% | 71.6–85.1 | 31 | 21.7% | 14.9–28.4 | 1.5 | 0.9–2.5 |
| Nationality** | |||||||||||
| Spanish | 689 | 83.1% | 80.6–85.7 | 544 | 79.0% | 75.9–82.0 | 145 | 21.0% | 18.0–24.1 | 2.8 | 1.4–3.1 |
| Foreign | 140 | 16.9% | 14.3–19.4 | 90 | 64.3% | 56.3–72.2 | 50 | 35.7% | 27.8–43.7 | 1 | |
| Religiosity | |||||||||||
| Yes, high commitment | 169 | 20.3% | 17.6–23.1 | 127 | 75.1% | 68.6–81.7 | 42 | 24.9% | 18.3–31.4 | 1.2 | 0.7–1.8 |
| Yes, practising | 218 | 26.2% | 23.2–29.2 | 173 | 79.4% | 74.0–84.7 | 45 | 20.6% | 15.3–26.0 | 0.9 | 0.6–1.4 |
| Yes, nonpractising | 250 | 30.1% | 27.0–33.2 | 195 | 78.0% | 72.9–83.1 | 55 | 22.0% | 16.9–27.1 | 1 | |
| No | 112 | 13.5% | 11.2–15.8 | 82 | 73.2% | 65.0–81.4 | 30 | 26.8% | 18.6–35.0 | 1.3 | 0.8–1.2 |
| Does not answer | 82 | 9.9% | 7.8–11.9 | 59 | 72.0% | 62.2–81.7 | 23 | 28.0% | 18.3–37.8 | 1.4 | 0.8–2.4 |
Abbreviations: CI, confidence interval; OR, odds ratio; SVE, secondary vocational education.
Table 2 summarises maternal knowledge and sources of information on the HPV vaccine. Of the surveyed mothers, 93.8% had heard of HPV infection, especially on television (71.5%), followed by the press (46.5%), the radio (26.3%) and the Internet (25.5%). None of these mass media had an effect on their decision to vaccinate or not vaccinate their daughters. In contrast, informational pamphlets, which were used by 55.5% of the mothers, did have an effect, increasing the prevalence of vaccination from 71.3% to 82.7% in mothers that had read them (OR, 1.9; 95% CI, 1.4–2.7).
Mass media and knowledge and beliefs on infection by HPV and their association with vaccination against HPV. Frequencies, percentages, 95% CI and bivariate logistic regression OR.
| Has heard of: | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | Vaccinated | Unvaccinated | Association | ||||||||
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | OR | 95% CI | |
| Infection by HPV | |||||||||||
| No | 52 | 6.2% | 3.1–7.9 | 35 | 67.3% | 54.6–80.1 | 17 | 32.7% | 19.9–45.4 | 1 | |
| Yes | 781 | 93.8% | 90.6–95.4 | 603 | 77.2% | 74.3–80.2 | 178 | 22.8% | 19.8–25.7 | 1.6 | 0.9–3.0 |
| HPV on television | |||||||||||
| No | 232 | 28.5% | 25.4–31.6 | 180 | 77.6% | 72.2–83.0 | 52 | 22.4% | 17.0–27.8 | 1.0 | 0.7–1.4 |
| Yes | 583 | 71.5% | 68.4–74.6 | 453 | 77.7% | 74.3–81.1 | 130 | 22.3% | 18.9–25.7 | 1 | |
| HPV in the press | |||||||||||
| No | 436 | 53.5% | 50.1–56.9 | 341 | 78.2% | 74.3–82.1 | 95 | 21.8% | 17.9–25.7 | 1.1 | 0.8–1.5 |
| Yes | 379 | 46.5% | 43.1–49.9 | 292 | 77.0% | 72.8–81.3 | 87 | 23.0% | 18.7–27.2 | 1 | |
| HPV on the radio | |||||||||||
| No | 601 | 73.7% | 70.7–76.8 | 462 | 76.9% | 73.5–80.2 | 139 | 23.1% | 19.8–26.5 | 1 | |
| Yes | 214 | 26.3% | 23.2–29.3 | 171 | 79.9% | 74.5–85.3 | 43 | 20.1% | 14.7–25.5 | 1.2 | 0.8–1.7 |
| HPV in the Internet | |||||||||||
| No | 607 | 74.5% | 71.5–77.5 | 479 | 78.9% | 75.7–82.2 | 128 | 21.1% | 17.8–24.3 | 1.3 | 0.9–1.9 |
| Yes | 208 | 25.5% | 22.5–28.5 | 154 | 74.0% | 68.1–80.0 | 54 | 26.0% | 20.0–31.9 | 1 | |
| HPV in informational pamphlets** | |||||||||||
| No | 363 | 44.5% | 41.1–48.0 | 259 | 71.3% | 66.7–76.0 | 104 | 28.7% | 24.0–33.3 | 1 | |
| Yes | 452 | 55.5% | 52.0–58.9 | 374 | 82.7% | 79.3–86.2 | 78 | 17.3% | 13.8–20.7 | 1.9 | 1.4–2.7 |
| HPV infection may cause | |||||||||||
| Liver cancer | |||||||||||
| No (Correct) | 820 | 98.4% | 97.6–99.3 | 626 | 76.3% | 73.4–79.3 | 194 | 23.7% | 20.7–26.6 | 1 | |
| Yes | 13 | 1.6% | 0.7–2.4 | 12 | 92.3% | 77.8–100 | 1 | 7.7% | 0.0–22.2 | 3.7 | 0.5–29 |
| Penile cancer | |||||||||||
| No | 789 | 94.7% | 93.2–96.2 | 605 | 76.7% | 73.7–79.6 | 184 | 23.3% | 20.4–26.3 | 1 | |
| Yes (Correct) | 44 | 5.3% | 3.8–6.8 | 33 | 75.0% | 62.2–87.8 | 11 | 25.0% | 12.2–37.8 | 1.1 | 0.5–2.2 |
| Ovarian cancer* | |||||||||||
| No (Correct) | 626 | 75.2% | 72.2–78.1 | 468 | 74.8% | 71.4–78.2 | 158 | 25.2% | 21.8–28.6 | 1 | |
| Yes | 207 | 24.8% | 21.9–27.8 | 170 | 82.1% | 76.9–87.3 | 37 | 17.9% | 12.7–23.1 | 1.5 | 1.0–2.3 |
| Genital warts | |||||||||||
| No | 675 | 81.0% | 78.4–83.7 | 515 | 76.3% | 73.1–79.5 | 160 | 23.7% | 20.5–26.9 | 1 | |
| Yes (Correct) | 158 | 19.0% | 16.3–21.6 | 123 | 77.8% | 71.4–84.3 | 35 | 22.2% | 15.7–28.6 | 1.1 | 0.7–1.6 |
| Cervical cancer | |||||||||||
| No | 17 | 2.0% | 1.1–3.0 | 14 | 82.4% | 64.2–100 | 3 | 17.6% | 0.0–35.8 | ||
| Yes (Correct) | 816 | 98.0% | 97.0–98.9 | 624 | 76.5% | 73.6–79.4 | 192 | 23.5% | 20.6–26.4 | 1.4 | 0.4–5.0 |
| Knowledge of VPH (overall) | |||||||||||
| Low | 718 | 86.2% | 83.9–88.5 | 550 | 76.6% | 73.5–79.7 | 168 | 23.4% | 20.3–26.5 | 1 | |
| High | 115 | 13.8% | 11.5–16.1 | 88 | 76.5% | 68.8–84.3 | 27 | 23.5% | 15.7–31.2 | 1.0 | 0.6–1.6 |
Abbreviations: CI, confidence interval; HPV, human papillomavirus; OR, odds ratio.
Overall, mothers had a low level of knowledge about HPV infections (86.2%). Of all mothers, 98.0% knew that HPV infection could cause cervical cancer, but 81.0% were not aware that it also causes genital warts and 94.7% that it can also cause penile cancer. The incorrect belief that HPV can cause ovarian cancer (24.8% of mothers) was associated with a higher frequency of vaccination in their daughters (OR, 1.5; 95% CI, 1.0–2.3).
Table 3 presents the data on the knowledge of HPV and the information received from health professionals along with the effect that they had on the decision to vaccinate.
Information given by health professionals and knowledge of HPV vaccine in association to vaccination against HPV. Frequencies, percentages, 95% CI and bivariate logistic regression OR.
| Total | Vaccinated | Unvaccinated | Association | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | OR | 95% CI | |
| Have you heard of the HPV vaccine | |||||||||||
| No | 52 | 6.2% | 3.1–7.9 | 35 | 67.3% | 54.6–80.1 | 17 | 32.7% | 19.9–45.4 | 1 | |
| Yes | 781 | 93.8% | 90.6–95.4 | 603 | 77.2% | 74.3–80.2 | 178 | 22.8% | 19.8–25.7 | 1.6 | 0.9–3.0 |
| I have been informed on the vaccine by | |||||||||||
| The paediatrician* | |||||||||||
| No | 341 | 41.8% | 38.5–45.2 | 240 | 70.4% | 65.5–75.2 | 101 | 29.6% | 24.8–34.5 | 1 | |
| Yes | 474 | 58.2% | 54.8–61.5 | 393 | 82.9% | 79.5–86.3 | 81 | 17.1% | 13.7–20.5 | 2.0 | 1.5–2.8 |
| The paediatric nurse* | |||||||||||
| No | 640 | 78.5% | 75.7–81.3 | 487 | 76.1% | 72.8–79.4 | 153 | 23.9% | 20.6–27.2 | 1 | |
| Yes | 175 | 21.5% | 18.7–24.3 | 146 | 83.4% | 77.9–88.9 | 29 | 16.6% | 11.1–22.1 | 1.6 | 1.0–2.4 |
| The family physician | |||||||||||
| No | 651 | 79.9% | 77.1–82.6 | 509 | 78.2% | 75.0–81.4 | 142 | 21.8% | 18.6–25.0 | 1.1 | 0.8–1.7 |
| Yes | 164 | 20.1% | 17.4–22.9 | 124 | 75.6% | 69.0–82.2 | 40 | 24.4% | 17.8–31.0 | 1 | |
| The gynaecologist | |||||||||||
| No | 545 | 67.6% | 64.4–70.8 | 420 | 77.1% | 73.5–80.6 | 134 | 24.6% | 21.0–28.2 | 1 | |
| Yes | 261 | 32.4% | 29.2–35.6 | 213 | 81.6% | 76.9–86.3 | 48 | 18.4% | 13.7–23.1 | 1.4 | 0.9–2.0 |
| Some type of health professional (total) | |||||||||||
| No | 175 | 21.5% | 18.7–24.3 | 113 | 64.6% | 57.5–71.7 | 62 | 35.4% | 28.3–42.5 | 1 | |
| Yes | 640 | 78.5% | 75.7–81.3 | 520 | 81.3% | 78.2–84.3 | 120 | 18.8% | 15.7–21.8 | 2.4 | 1.6–3.4 |
| How many doses does vaccination require?** | |||||||||||
| Incorrect | 72 | 8.6% | 6.7–10.6 | 21 | 29.2% | 18.7–39.7 | 51 | 70.8% | 60.3–81.3 | 1 | |
| Correct (3) | 761 | 91.4% | 89.4–93.3 | 617 | 81.1% | 78.3–83.9 | 144 | 18.9% | 16.1–21.7 | 10 | 6.1–18 |
| The vaccine protects against | |||||||||||
| Liver cancer | |||||||||||
| No (correct) | 827 | 99.3% | 98.7–99.9 | 633 | 76.5% | 73.7–79.4 | 194 | 23.5% | 20.6–26.3 | 1 | |
| Yes | 6 | 0.7% | 0.1–1.3 | 5 | 83.3% | 53.5–100 | 1 | 16.7% | 0.0–46.5 | 1.5 | 0.2–13 |
| Penile cancer | |||||||||||
| No | 805 | 96.6% | 95.4–97.9 | 617 | 76.6% | 73.7–79.6 | 188 | 23.4% | 20.4–26.3 | 1.1 | 0.4–2.6 |
| Yes (correct) | 28 | 3.4% | 2.1–4.6 | 21 | 75.0% | 59.0–91.0 | 7 | 25.0% | 9.0–41.0 | 1 | |
| Ovarian cancer | |||||||||||
| No (correct) | 652 | 78.3% | 75.5–81.1 | 491 | 75.3% | 72.0–78.6 | 161 | 24.7% | 21.4–28.0 | 1 | |
| Yes | 181 | 21.7% | 18.9–24.5 | 144 | 79.6% | 73.7–85.4 | 34 | 18.8% | 13.1–24.5 | 1.4 | 0.9–2.1 |
| Genital warts | |||||||||||
| No | 703 | 84.4% | 81.9–86.9 | 535 | 76.1% | 72.9–79.3 | 168 | 23.9% | 20.7–27.1 | 1 | |
| Yes (correct) | 130 | 15.6% | 13.1–18.1 | 103 | 79.2% | 72.3–86.2 | 27 | 20.8% | 13.8–27.7 | 1.2 | 0.7–1.9 |
| Cervical cancer | |||||||||||
| No | 18 | 2.2% | 1.2–3.1 | 12 | 66.7% | 44.9–88.4 | 6 | 33.3% | 11.6–55.1 | 1 | |
| Yes (correct) | 815 | 97.8% | 96.9–98.8 | 626 | 76.8% | 73.9–79.7 | 189 | 23.2% | 20.3–26.1 | 1.6 | 0.6–4.5 |
| Knowledge of HPV vaccine | |||||||||||
| Low | 742 | 89.1% | 87.0–91.2 | 564 | 76.0% | 72.9–79.1 | 178 | 24.0% | 20.9–27.1 | 1 | |
| High | 91 | 10.9% | 8.8–13.0 | 74 | 81.3% | 73.3–89.3 | 17 | 18.7% | 10.7–26.7 | 1.4 | 0.8–2.4 |
Abbreviations: CI, confidence interval; HPV, human papillomavirus; OR, odds ratio.
In our sample, 93.8% of the mothers had heard of the vaccine. The information given to mothers by different types of health professionals had different effects: 58.2% of the mothers received information from the paediatrician, which had a favourable effect on vaccination (OR, 2.0; 95% CI, 1.5–2.8), while a lower percentage of 21.5% received information from the nurse that also had a favourable affected on vaccination (OR: 1.6; 95% CI, 1.0–2.4). However, neither the advice of family physicians nor that of gynaecologists seemed to have an effect on the mothers’ decision to vaccinate their daughters. In our sample, 78.5% of the mothers received advice from at least one type of the health professionals under consideration, and the advice had a positive effect on vaccination (OR, 2.4; 95% CI, 1.6–3.4).
The level of knowledge about HPV was low in 89.1% of the mothers. While 91.4% knew the correct dosage, 97.8% knew that the vaccine protects against cervical cancer, 99.3% knew the vaccine does not protect against liver cancer and 78.3% that it does not protect against ovarian cancer, 96.6% did not know that the vaccine protects against penile cancer and 84.4% that it protects against genital warts. We found a strong association between mothers knowing the exact number of doses and having chosen to vaccinate their daughters (OR, 10; 95% CI, 6.1–18).
Table 4 summarises other factors associated with vaccination against HPV. It shows that maternal attendance of routine checkups with a gynaecologist was associated with a higher rate of vaccination in their daughters compared to daughters of mothers that do not go to the gynaecologist (OR, 1.9; 95% CI, 1.2–2.9). A higher acceptance of mothers of vaccines as a method of disease prevention was associated with a higher percentage of vaccinated daughters (OR, 3.8; 95% CI, 3.0–4.7). The perception of mothers of being at risk of having an HPV infection (10.9%) was associated with a significant increase in vaccination of their daughters (OR, 1.6; 95% CI, 1.1–2.4). Of the 10 concerns under study, cancer ranked highest, with 94.5% of mothers responding that it worried them moderately or a lot, and STDs ranked eighth, with 68.1% of mothers expressing worry.
Other factors associated with vaccination against HPV.
| Total | Vaccinated | Unvaccinated | Association | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | OR | 95% CI | |
| Visit to gynaecologist, reason** | |||||||||||
| Routine checkups | 606 | 72.7% | 69.7–75.8 | 477 | 78.7% | 75.5–82.0 | 129 | 21.3% | 18.0–24.5 | 1.9 | 1.2–2.9 |
| Other reasons | 104 | 12.5% | 10.2–14.7 | 80 | 76.9% | 68.8–85.0 | 24 | 23.1% | 15.0–31.2 | 1.7 | 0.9–3.1 |
| Does not visit | 123 | 14.8% | 12.4–17.2 | 81 | 65.9% | 57.5–74.2 | 42 | 34.1% | 25.8–42.5 | 1 | |
| Acceptance of vaccination as a means to prevent diseases*** | |||||||||||
| Very in favour | 306 | 36.7% | 33.5–40.0 | 272 | 88.9% | 85.4–92.4 | 34 | 11.1% | 7.6–14.6 | 52 | 23–119 |
| Quite in favour | 394 | 47.3% | 43.9–50.7 | 333 | 84.5% | 80.9–88.1 | 61 | 15.5% | 11.9–19.1 | 35 | 16–78 |
| Indifferent | 49 | 5.9% | 4.3–7.5 | 25 | 51.0% | 37.0–65.0 | 24 | 49.0% | 35.0–63.0 | 7.0 | 2.7–17 |
| Not in favour | 60 | 7.2% | 5.4–9.0 | 8 | 13.3% | 4.7–21.9 | 52 | 86.7% | 78.1–95.3 | 1 | |
| Opposeda | 24 | 2.9% | 1.7–4.0 | 0 | 0.0% | 0.0–0.0 | 24 | 100% | 100–100 | 3.8b,* | 3.0–4.7 |
| Do you think you are at risk of having an HPV infection?** | |||||||||||
| No | 577 | 89.1% | 87.0–91.2 | 428 | 76.0% | 72.9–79.1 | 149 | 24.0% | 20.9–27.1 | 1 | |
| Yes | 247 | 10.9% | 8.8–13.0 | 204 | 81.3% | 73.3–89.3 | 43 | 18.7% | 10.7–26.7 | 1.6 | 1.1–2.4 |
| Assessment of concerns. Category shown: “It worries me moderately or a lot”. Reference category “It worries me a little or not at all” | |||||||||||
| Weight problems | 514 | 61.7% | 58.4–65.0 | 391 | 61.3% | 57.5–65.1 | 123 | 63.1% | 56.3–69.9 | 0.9 | 0.7–1.3 |
| Emerging epidemics | 524 | 62.9% | 59.6–66.2 | 394 | 61.8% | 58.0–65.5 | 130 | 66.7% | 60.1–73.3 | 0.8 | 0.6–1.1 |
| STDs | 567 | 68.1% | 64.9–71.2 | 430 | 67.4% | 63.8–71.0 | 137 | 70.3% | 63.8–76.7 | 0.9 | 0.6–1.2 |
| Environmental risks | 569 | 68.3% | 65.1–71.5 | 441 | 69.1% | 65.5–72.7 | 128 | 65.6% | 59.0–72.3 | 1.2 | 0.8–1.6 |
| AIDS | 644 | 77.3% | 74.5–80.2 | 500 | 78.4% | 75.2–81.6 | 144 | 73.8% | 67.7–80.0 | 1.3 | 0.9–1.9 |
| Terrorism | 657 | 78.9% | 76.1–81.6 | 502 | 78.7% | 75.5–81.9 | 155 | 79.5% | 73.8–85.2 | 1.0 | 0.6–1.4 |
| Crime and violence | 714 | 85.7% | 83.3–88.1 | 547 | 85.7% | 83.0–88.5 | 167 | 85.6% | 80.7–90.6 | 1.0 | 0.6–1.6 |
| Traffic accidents | 749 | 89.9% | 87.9–92.0 | 577 | 90.4% | 88.2–92.7 | 172 | 88.2% | 83.7–92.7 | 1.3 | 0.8–2.1 |
| Unemployment/school failure | 778 | 93.4% | 91.7–95.1 | 601 | 94.2% | 92.4–96.0 | 177 | 90.8% | 86.7–94.8 | 1.7 | 0.9–3.0 |
| Cancer | 787 | 94.5% | 92.9–96.0 | 608 | 95.3% | 93.7–96.9 | 179 | 91.8% | 87.9–95.6 | 1.8 | 1.0–3.4 |
Abbreviations: CI, confidence interval; HPV, human papillomavirus; OR, odds ratio; STDs, sexually transmitted diseases.
In the 195 mothers of daughters that had not been vaccinated against HPV (Table 5), the main reasons not to vaccinate were fear of adverse effects (45.6%) and lack of information (11.8%). When daughters had not been vaccinated, the primary decision-maker had been the mother in 48.2% of the cases, and the daughter in 30.3%. There was no secondary decision-maker in 60.5% of cases, and the secondary decision-maker was the mother in 16.2% and the mother's partner in 11.8% of cases. When it came to the advice received by health professionals by mothers of unvaccinated daughters, 24.6% of mothers had not had a discussion with a health professional, and 36.9% had received information but not guidance, while 22.1% had been advised to vaccinate their daughters. Only 15.9% were advised by a health professional not to vaccinate.
Reasons not to vaccinate, primary decision-maker and professional advice.
| N=195 | % | 95% CI | |
|---|---|---|---|
| Reasons not to vaccinate | |||
| My doctor said it was not necessary | 8 | 4.1% | 1.3–6.9 |
| I will have her vaccinated in a few weeks | 10 | 5.1% | 2.0–8.2 |
| She has received some doses of the vaccine and the last one is pending | 3 | 1.5% | 0.0–3.3 |
| I’d rather wait | 20 | 10.3% | 6.0–14.5 |
| I don’t want this vaccine because I don’t think it is necessary | 15 | 7.7% | 4.0–11.4 |
| I’m worried about adverse effects | 89 | 45.6% | 38.6–52.6 |
| I don’t believe in vaccination | 4 | 2.1% | 0.1–4.0 |
| I have not been given enough information on this vaccine | 23 | 11.8% | 7.3–16.3 |
| I don’t know | 23 | 11.8% | 7.3–16.3 |
| The primary decision-maker in the choice not to vaccinate was | |||
| My daughter | 59 | 30.3% | 23.8–36.7 |
| Myself | 94 | 48.2% | 41.2–55.2 |
| My partner | 1 | 0.5% | 0.0–1.5 |
| My doctor/paediatrician | 12 | 6.2% | 2.8–9.5 |
| The paediatric nurse | 1 | 0.5% | 0.0–1.5 |
| My friends | 1 | 0.5% | 0.0–1.5 |
| Others | 20 | 10.3% | 6.0–14.5 |
| I don’t know | 7 | 3.6% | 1.0–6.2 |
| The secondary decision-maker in the choice not to vaccinate was | |||
| Myself | 32 | 16.4% | 11.2–21.6 |
| My partner | 23 | 11.8% | 7.3–16.3 |
| My doctor/paediatrician | 10 | 5.1% | 2.0–8.2 |
| My friends | 3 | 1.5% | 0.0–3.3 |
| Others | 9 | 4.6% | 1.7–7.6 |
| There was no secondary decision-maker | 118 | 60.5% | 53.7–67.4 |
| Regarding the advice given by your doctor or nurse | |||
| I have not talked to them | 48 | 24.6% | 18.6–30.7 |
| They advised me to vaccinate | 43 | 22.1% | 16.2–27.9 |
| They gave me information but left the decision about vaccination to me | 72 | 36.9% | 30.1–43.7 |
| They have advised that I do not give her the vaccine or that I defer giving it | 31 | 15.9% | 10.8–21.0 |
| I don’t know | 1 | 0.5% | 0.0–1.5 |
Table 6 shows the logistic regression model of vaccination versus nonvaccination of daughters with adjusted ORs. We can see that a very favourable perception of vaccination as a preventive measure was associated with a higher vaccination frequency (OR, 4.1; 95% CI, 3.3–5.3). The adjusted OR for mothers of Spanish nationality was 2.2 (95% CI, 1.3–3.6), while the adjusted OR for mothers that were married or in a domestic partnership was 2.0 (95% CI, 1.2–3.3). When it came to the information and advice received by mothers, informational pamphlets (OR, 2.0; 95% CI, 1.4–3.1) and advice given at the paediatrics clinic by either the nurse or the paediatrician had promoted vaccination, showing adjusted ORs of 2.1 (95% CI, 1.2–3.4) and 1.8 (95% CI, 1.2–2.8), respectively.
Logistic regression model of vaccination against HPV. Adjusted OR and 95% CI for variables that reached statistical significance in the model.
| Group with most significant willingness to vaccinate | 95% CI | ||
|---|---|---|---|
| Sig | OR | ||
| Married or in domestic partnership | .002 | 2.2 | 1.3–3.6 |
| Spanish nationality | .008 | 2.0 | 1.2–3.3 |
| Approves of vaccines as preventive method | .000 | 4.1 | 3.3–5.3 |
| Advised by paediatrician | .004 | 1.8 | 1.2–2.8 |
| Informed by informational pamphlets | .001 | 2.0 | 1.4–3.1 |
| Advised by paediatric nurse | .006 | 2.1 | 1.2–3.4 |
| Constant | .000 | 0.03 | |
Abbreviations: CI, confidence interval; HPV, human papillomavirus; OR, odds ratio; Sig, statistical significance.
In our study, three out of four girls were vaccinated, which is not enough for the success of a vaccination programme aimed at achieving herd immunity to a virus with a very high prevalence as is HPV.9,10 Our analysis of demographic variables showed that the mothers most willing to vaccinate their daughters were mothers that were married or in a domestic partnership, older mothers, mothers with secondary vocational training and mothers of Spanish nationality. On the other hand, religion had no influence on the decision.
When we analysed the influence of the mass media, we found that only informational pamphlets had a moderate positive influence on the willingness to vaccinate.
The maternal level of knowledge about HPV was low. While a high percentage had heard about HPV and were aware of its association with cervical cancer, it was not known that it can also cause penile cancer or genital warts. Furthermore, one fourth of the mothers incorrectly associated HPV with ovarian cancer. This false belief was associated with a greater willingness to vaccinate. The maternal level of knowledge about the HPV vaccine was also low. Most mothers had heard of the vaccine and even knew the number of doses required for vaccination, but they did not know exactly which types of cancers and symptoms can be prevented by the vaccine.
The reach of the information provided to mothers by health professionals was modest, but the information was very effective, as it was associated with a higher vaccination frequency. The results emphasised the role of the paediatrician and the nurse in providing information.
Mothers that visited the gynaecologist for routine checkups were more likely to have their daughters vaccinated, as did mothers that perceived a greater risk of having a HPV infection.
The belief in vaccination as a health prevention method was strongly correlated with a greater willingness to vaccinate, as the more mothers trusted vaccines the higher the vaccination coverage in their daughters.
We found that a high percentage of participants had refused vaccination, and the main reasons for this refusal were fear of adverse effects and lack of information. The decision not to vaccinate was most frequently taken by the mother or the daughter. In these cases, the advice of health professionals was either inconsistent or nonexistent.
The predictive logistic model showed that a favourable perception of vaccination had a strong effect, as did professional advice and informational pamphlets. The sociodemographic control variables entered in the model were marital status and nationality.
The situation we have described does not differ significantly from the descriptions of studies conducted in other countries, in which the willingness to vaccinate ranged between 80%11 and 64%,12 figures similar to those obtained in our study that in turn are similar to those found in studies conducted in other areas of Spain.13 This results stand in contrast to the high acceptance rates found in the period preceding the licensing of the vaccine, which reached up to 90%.14
The limited influence of sociodemographic variables was consistent with the findings of other studies.11,15–19 Our results were also similar to those of a study conducted in Sweden20 that found a lower willingness to vaccinate in foreign parents, and especially those not from the European Union. We did not take into account household income or social class because vaccination against HPV is free as part of the routine immunisation schedule.21
While in our study married women were most willing to vaccinate their daughters, in a study conducted in Canada single parents were the most willing.22 This discrepancy may be due to single parents possibly being more aware of the risk of infection by HPV, something that was not addressed by the Canadian study and that was associated with a higher acceptance of the vaccine in ours.
The mass media did not have a significant effect on decision-making in the period under study, although it did contribute to the widespread awareness of HPV and the vaccine against it.12,17,23 The concerns raised by the mass media give added value to the information provided by health professionals12,22–24 and educational pamphlets.11 When we consider the extent of the media coverage devoted to the two adverse effect cases in 2009, professional advice becomes all the more valuable.
The public has a very favourable view of vaccines, a fact that is correlated to the willingness to accept new vaccines. The response to the HPV vaccine has been consistent with this fact,15,16,18,19,22 as was also evinced in this study. However, these populations tend to have little knowledge of the HPV vaccine and the diseases that it prevents. Nevertheless, there is no clear evidence of a significant association between this knowledge and the willingness to vaccinate,14,15,22 and when such evidence has been found, it has suggested that a higher willingness to vaccinate is associated with a lower level of knowledge.17 Lack of information is one of the main reasons for not vaccinating12,14 along with fear of adverse effects.12,13,15,20,25
Although this study had a high participation rate compared to similar research,11,14,17–19 its results should be extrapolated to other populations with caution. Some aspects were not covered by the survey, such as the mother's history of STDs.26 On the other hand, one of the strengths of the study is that it reached a wide spectrum of the population, encompassing public and private schools, and that it was designed to be representative of urban as well as rural areas.
The mass media has contributed to disseminating knowledge about HPV, although a decisive role cannot be attributed to it in shaping the willingness to vaccinate. On the contrary, professional advice had the most influence in the decision to vaccinate, although this advice has not reached all mothers of girls of vaccination age, and in some cases the advice has been against vaccinating. Thus, there had been missed opportunities for delivering professional advice. Increasing the involvement of health professionals to facilitate a more direct flow of information may lead to higher coverage rates, considering that there is a broad margin for improvement. On the other hand, increasing the public trust in vaccination is key to achieving greater willingness to vaccinate.
FundingThe study received a research grant from Sanofi-Pasteur MSD.
Conflicts of interestThe authors Diez-Domingo J and Puig-Barberá J have participated in clinical trials sponsored by Glaxo-Smith-Klein (GSK) and Sanofi Pasteur MSD. The rest of the authors have no conflicts of interest to declare.
Please cite this article as: Navarro-Illana P, Caballero P, Tuells J, Puig-Barberá J, Diez-Domingo J. Aceptabilidad de la vacuna contra el virus del papiloma humano en madres de la provincia de Valencia (España). An Pediatr (Barc). 2015;83:318–327.