Neonatal hypocalcaemia is a common and potentially severe metabolic disorder of variable aetiology. Vitamin D deficiency (VDD) has been described as a cause of neonatal late-onset hypocalcaemia (NLOH). We describe our experience with 2 cases of neonatal early-onset hypocalcaemia (NEOH) associated with neonatal and maternal VDD.
Case 1: newborn girl that developed pathologic tremors at 40 h post birth. The mother was of European ascent exposed to sunlight less than 30 min a day. The patient was born in March at 38 weeks of gestation with a birth weight 3590 g in an uncomplicated vaginal delivery. Testing found serum levels of ionized calcium of 4.2 mg/dL, total calcium of 8.1 mg/dL and vitamin D of 14 ng/mL. The infant was given calcium gluconate 10% orally at a dose of 2 mL/kg/day, which improved the clinical manifestations. Testing in the mother found levels of vitamin D of 13 ng/mL and of parathyroid hormone (PTH) of 82.8 pg/mL (15–65 pg/mL).
Case 2: newborn boy that exhibited hypotonia and lethargy at 48 h post birth. The mother was of Arabic ancestry with no exposure to sunlight. The boy was born in February in an uncomplicated delivery at 40 weeks of gestation, with a birth weight of 3180 g. He had serum levels of ionized calcium of 3.27 mg/dL, total calcium of 8.2 mg/dL and vitamin D of 7.1 ng/mL. Calcium gluconate 10% was administered to the patient by the oral route at a dose of 2 mL/kg/day, which improved the clinical manifestations. The mother had serum levels of vitamin D of 4.2 ng/mL, of PTH of 57.9 pg/mL, of total calcium of 8 mg/dL and of phosphorus of 2.5 mg/dL.
Both mothers resided in Teruel (latitude, 40.25°) and had a skin phototype of 1–2 in the Fitzpatrick scale, a low level of physical activity (took some walks each week) and a body mass index under 30 kg/m2, and neither was taking vitamin D. Both mothers were treated successfully with calcifediol supplementation.
Tremors are the most frequent paroxysmal manifestations in the neonatal period, and hypotonia and lethargy are nonspecific symptoms found in neonatal metabolic disorders. They must be assessed as early warning signs of disorders like hypocalcaemia and VDD.1
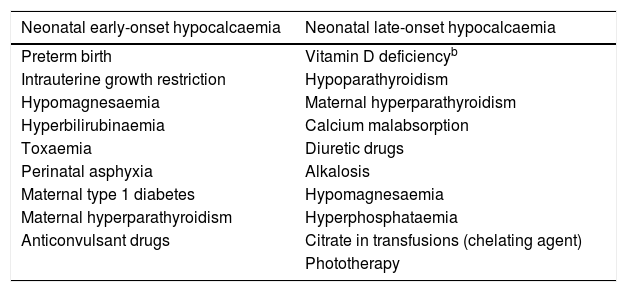
The main symptoms of neonatal hypocalcaemia are agitation, tremors, lethargy, seizures, changes in muscle tone, stridor or prolongation of the QTc interval (>0.4 ms). A distinction is made between NEOH (the first 3–4 days of life) and NLOH (the next 5–10 days) (Table 1). Historically, vitamin D deficiency has not been considered a cause of NEOH. The evidence shows a probable association between ethnicity, maternal vitamin D levels and neonatal serum calcium levels,2 so that maternal vitamin D levels and neonatal calcium levels may vary depending on the maternal phototype or cultural factors, and previous data suggest that higher supplementation doses may have a positive impact on the infant, including on calcium levels (Table 2).3
Causes of neonatal hypocalcaemia.a
| Neonatal early-onset hypocalcaemia | Neonatal late-onset hypocalcaemia |
|---|---|
| Preterm birth | Vitamin D deficiencyb |
| Intrauterine growth restriction | Hypoparathyroidism |
| Hypomagnesaemia | Maternal hyperparathyroidism |
| Hyperbilirubinaemia | Calcium malabsorption |
| Toxaemia | Diuretic drugs |
| Perinatal asphyxia | Alkalosis |
| Maternal type 1 diabetes | Hypomagnesaemia |
| Maternal hyperparathyroidism | Hyperphosphataemia |
| Anticonvulsant drugs | Citrate in transfusions (chelating agent) |
| Phototherapy |
Neonatal hypocalcaemia: serum total calcium <8 mg/dL (2 mmol/L) or ionized calcium <4.4 mg/dL (1.1 mmol/L), in term neonates and preterm neonates with birth weights greater than 1500 g, and total calcium <7 mg/dL (1.75 mmol/L) or ionised calcium <4 mg/dL (1 mmol/L) in very low birth weight neonates or neonates weighing <1500 g.
Benefits of isolated vitamin D supplementation found in systematic reviews.
| Benefits described by Harvey et al. | ||
|---|---|---|
| Birth weight | Observational | Combined regression coefficient, 5.63 g/10% of maternal vitamin D; 95% CI, 1.11–10.16 ga |
| Birth bone mass | Observational | 5 of 8 OSs found a statistically significant association |
| Neonatal serum calcium levels | Meta-analysis | DM, 0.05 mmol/L; 95% CI, 0.02–0.05 mmol/La |
| Benefits described by Palacios et al. | ||
|---|---|---|
| Preeclampsia | Meta-analysis | RR, 0.48; 95% CI, 0.30–0.79; 4 RCTsa |
| Gestational diabetes | Meta-analysis | RR, 0.51; 95% CI, 0.27–0.97; 4 RCTsa |
| Low birth weight | Meta-analysis | RR, 0.55; 95% CI, 0.35–0.87; 5 RCTsa |
| Severe postpartum haemorrhage | Meta-analysis | RR, 0.68; 95% CI, 0.51–0.91; 1 RCTa |
| Preterm birth (< 37 W G) | Meta-analysis | RR, 0.66; 95% CI, 0.34–1.30; 7 RCTs |
CI, confidence interval; DM, difference of means; OS, observational study; RCT, randomised clinical trial; RR, relative risk; WG, weeks of gestation.
In Spain, one study found that even with multivitamin supplementation including 200 IU/day of vitamin D, 63% of pregnant women have insufficient vitamin D levels and 26% deficient levels.4 Another study found levels under 20 ng/mL in 64.4% of mothers and 41.3% of neonates and identified multiple gestation and non-European ethnicity as risk factors for hypovitaminosis D, and maternal supplementation, physical activity and sunlight exposure as protective factors.5 Although VDD is very prevalent and underdiagnosed, the authors of systematic reviews with meta-analysis have been cautious in recommending isolated vitamin D supplementation during pregnancy, as the potential relationship of this practice with preterm birth has not been well established, although the relative risk is less than 1 and not statistically significant (Table 2).6
Given the above, and taking into account that the immigrant population in Spain is growing, we recommend suspecting VDD as a possible cause of neonatal hypocalcaemia, whether of early or late onset, routine screening of pregnant women for VDD and isolated vitamin D supplementation on a case-by-case basis based on the results, as the potential benefits to pregnant women and infants seems to outweigh the risks.
Please cite this article as: Adán Lanceta V, Martín Ruiz N, Benito Costey S, Alijarde Lorente R, Martínez de Zabarte Fernández JM. Hipocalcemia neonatal precoz por déficit de vitamina D materna. Replanteando la suplementación. An Pediatr (Barc). 2022;96:153–154.