Early in the coronavirus disease 2019 (COVID-19) pandemic, it was recommended that rooming-in and breastfeeding (BF)1 be avoided in mothers infected by SARS-CoV-2. Although later guidelines recommended maintaining early mother-infant contact and BF promotion (World Health Organization and Sociedad Española de Neonatología [SENeo]),2 in many instances, the pressure on the health care system and the reorganization of care delivery hindered adherence to these recommendations.3
The primary objective of our study was to assess whether the exclusive BF rate during the stay in the maternity ward and at discharge were affected by the detection of SARS-CoV-2 infection in the mother at the time of delivery in tertiary hospitals accredited by the baby-friendly hospital initiative (BFHI/IHAN). The secondary objective was to assess changes in exclusive BF rates through the first 3 waves of the pandemic in neonates born to mothers with SARS-CoV-2 infection.
We conducted a retrospective cohort study in a BFHI-accredited tertiary care hospital. The sample included mothers with a diagnosis by polymerase chain reaction (PCR) of infection by SARS-CoV-2 at the time of delivery (n = 58) who did not meet the exclusion criteria: admission to the intensive care unit (ICU), admission of newborn to neonatal ward for reasons unrelated to care organization, preterm birth or multiple pregnancy. The study also included a control group of mothers without SARS-CoV-2 infection (n = 116) who gave birth before and after each included mother, applying the same exclusion criteria. The study period included the first 3 waves of the pandemic.4 The sample included 84 patients in the first wave (28 with COVID-19 and 56 controls), 69 patients in the second wave (23 with COVID-19 and 46 controls) and 21 patients in the third wave (7 with COVID-19 and 14 controls). The study was approved by the research ethics committee.
We performed a descriptive analysis summarising categorical variables as absolute and relative frequencies and quantitative values as mean and standard deviation or median and interquartile range. In the univariate analysis, we used the Mann-Whitney U test or the Student t test to compare quantitative data and the chi square or Fisher exact test for hypothesis testing with categorical data. We set the level of significance at 0.05.
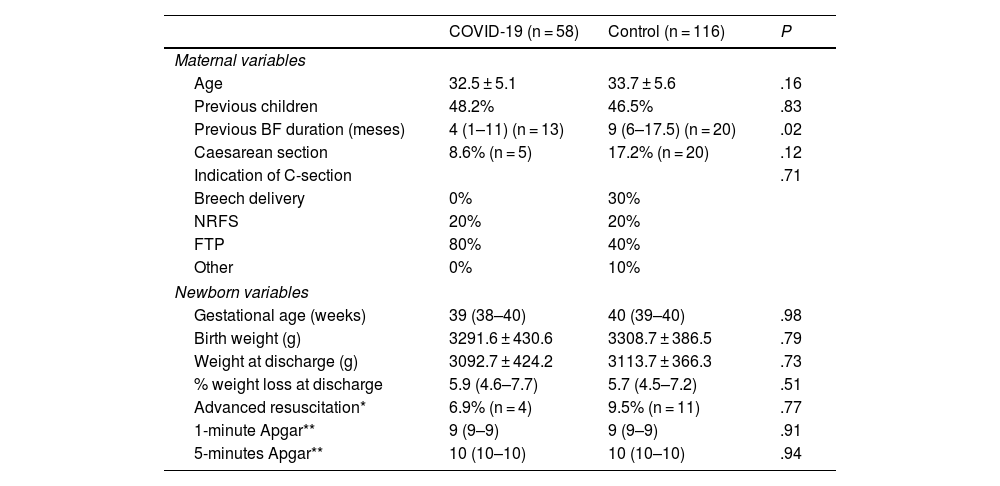
Table 1 presents the demographic characteristics of the 2 groups. We did not find differences in any variable other than the duration of BF in mothers that had previous children.
Demographic characteristics of the sample under study. Values given as mean ± standard deviation or median (interquartile range).
| COVID-19 (n = 58) | Control (n = 116) | P | |
|---|---|---|---|
| Maternal variables | |||
| Age | 32.5 ± 5.1 | 33.7 ± 5.6 | .16 |
| Previous children | 48.2% | 46.5% | .83 |
| Previous BF duration (meses) | 4 (1–11) (n = 13) | 9 (6–17.5) (n = 20) | .02 |
| Caesarean section | 8.6% (n = 5) | 17.2% (n = 20) | .12 |
| Indication of C-section | .71 | ||
| Breech delivery | 0% | 30% | |
| NRFS | 20% | 20% | |
| FTP | 80% | 40% | |
| Other | 0% | 10% | |
| Newborn variables | |||
| Gestational age (weeks) | 39 (38–40) | 40 (39–40) | .98 |
| Birth weight (g) | 3291.6 ± 430.6 | 3308.7 ± 386.5 | .79 |
| Weight at discharge (g) | 3092.7 ± 424.2 | 3113.7 ± 366.3 | .73 |
| % weight loss at discharge | 5.9 (4.6–7.7) | 5.7 (4.5–7.2) | .51 |
| Advanced resuscitation* | 6.9% (n = 4) | 9.5% (n = 11) | .77 |
| 1-minute Apgar** | 9 (9–9) | 9 (9–9) | .91 |
| 5-minutes Apgar** | 10 (10–10) | 10 (10–10) | .94 |
BF, breastfeeding; FTP, failure to progress; NRFS, nonreassuring fetal status.
The rate of exclusive BF in the maternity ward in infants born to mothers with a diagnosis of SARS-CoV-2 infection at the time of delivery was 72.4%, compared to 88.8% in the control group (OR, 0.33; 95% confidence interval [CI], 0.14−0.74; P = .004). At the time of discharge, the rate of exclusive BF in the group with SARS-CoV-2 infection was 70.7% compared to 86.2% in the control group (OR, 0.38; 95% CI, 0.17−0.83; P = .01).
When we compared exclusive BF rates in the first wave versus subsequent waves, we did not find differences in the rate during the hospital stay in the first wave versus the second and third waves (73.3% vs 71.4%; P = .87). There were also no differences in the exclusive BF rate at discharge (70% in first wave vs 71.4% in subsequent waves; P = .9).
In our study, we found that the rate of exclusive BF, both during the hospital stay and at discharge, was lower in women with a diagnosis of SARS-CoV-2 infection at the time of delivery compared to uninfected mothers.
A study that assessed the impact on exclusive BF rates during the first wave of the pandemic found a rate of 70.3% compared to 86.3% in a historical control group,5 results that are similar to ours. However, that study did not take into account maternal SARS-CoV-2 infection status.
The study has the limitations intrinsic to retrospective designs. In addition, the characteristics of the hospital in which it was conducted may limit the external validity of its findings.
In our area, exclusive BF rates were affected by infection by SARS-CoV-2. In the group of mothers with SARS-CoV-2 infection, we did not find any differences in the exclusive BF rates between the different waves of the pandemic.
We thank Dr Ana Royuela Vicente, who carried out the statistical analysis (Clinical Biostatistics Unit at the Instituto de Investigación Sanitaria Puerta de Hierro-Segovia of Arana).
Please cite this article as: Marín Gabriel MA, Manchado Perero S, Manzanares Gutiérrez L, Martín Lozoya S, Gómez de Olea Abad B. Infección por COVID-19 en el parto y tasas de lactancia materna exclusiva en una maternidad IHAN. An Pediatr (Barc). 2022;97:211–212.